During times of national crisis, a “chaotic assemblage of understandings” often coalesces around a singular event, especially one so devastating as the massacre of 49 people at the hands of a single gunman. It is no surprise that one of deadliest mass shootings in American history has provoked some of the most polarizing public debates about gun control and domestic terrorism. Yet far too often marginalized in recent discussions are those most affected by this incident: LGBTQ people and their spaces. Despite the vast outpouring of support across social media and major news networks, the precariousness of queer lives, especially of people of color, in the United States still remains persistently sidelined or even erased. As Salvador Vidal-Ortiz writes in his moving essay about the Orlando tragedy’s implications for queer latin@s, “to pay one’s respects for others’ losses, however, does not mean that we think of those lost as equals.” Empathy, he reminds us, is simply not enough when queer lives are threatened even in spaces meant to be safe for them.
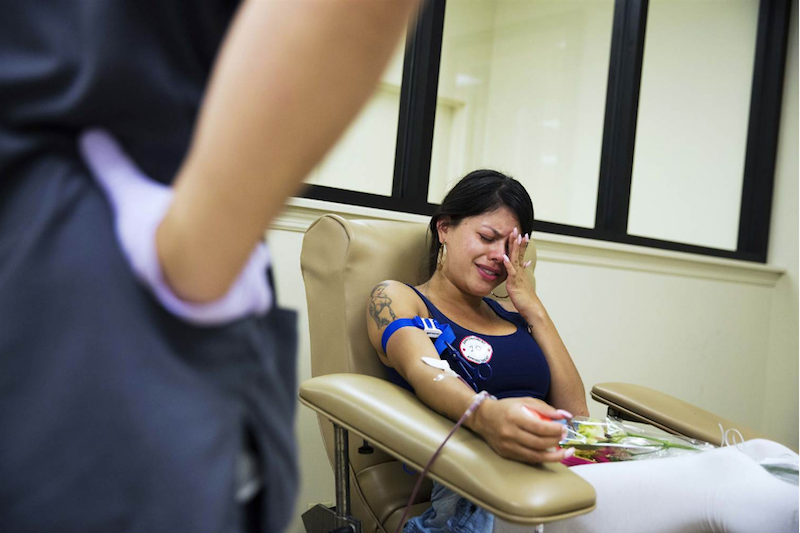
In the immediate wake of the shooting, members of the Orlando community rallied to provide one of the primary means of aid for gunshot victims in the United States: blood donation. However, many of these potential donors, particularly those who identified as gay men, could not support their own community members due to the enduring restrictions on blood donation for men who have sex with men (MSM). In the first iteration of these restrictions in 1983, the FDA refused blood from male donors who had had sexual contact with another male, even once, since 1977. Though the FDA’s recommendations have recently changed from indefinite deferral for MSM to a 12 month blood donor deferral since last MSM contact, blood donation policies still seem to hinge on a slippery conception of sexual behavior rather than on scientifically-justified risk. We must remember that still deferred indefinitely are any HIV-positive individuals, sex workers, IV drug users while heterosexual individuals who may be engaging in equally risky sexual behavior are free to donate. Given that such policies do not match up with current medical technologies (i.e. Nucleic Acid Testing), which accurately and reliably detect potential contaminants well before blood products are disseminated,[6] some key questions remain: 1) which individuals are privileged with the right to donate blood? 2) what is actually at stake in continuing to gatekeep blood donation?
Related article: “PRIDE, MINORITY STATUS, AND MASS SHOOTINGS“
In the Photo: Tatiana Osorio Photo Credit: NBC News
First reported in the CDC’s Morbidity and Mortality Weekly Report in 1982 as an “unexpected cluster of cases,” AIDS was described early on as “gay-related immune deficiency” (GRID) or more colloquially, “gay cancer” before being renamed “AIDS-related complex” (ARC) and finally “acquired immunodeficiency syndrome” (AIDS). As the LGBTQ community struggled to make sense of an epidemic that struck quickly and violently, many gay men died due to the negligence of both the national government and the medical establishment. Susan Sontag, writing in the peak of the epidemic, argued in AIDS and Its Metaphors (1989) that the pathologization of the “4 H’s” (“homosexuals,” “hemophiliacs,” “Haitians,” “hookers”) depended on a reductive logic that damned each group as a “tainted community that illness has judged.”[7] During this “epidemic of signification”[8] that proliferated alongside HIV, archaic notions of plague as punishment for societal “ills” took hold. Such panic was only exacerbated by the catastrophic contamination of blood products in the 70s through the mid-80s that resulted in the HIV infection of many hemophiliacs who had undergone blood transfusion.
Nowadays, several HIV Prevention and awareness programs have been launched globally to help and protect people living with HIV and to lower the chances of at-risk individuals of being infected.
For a full mindmap containing additional related articles and photos, visit #Orlando
The scapegoating of certain individuals as privileged carriers of the virus and “risk groups” as those in need of regulation or even extermination still underpins the FDA’s blood donation policies.[9] The continued deferral of blood donations from gay men who may be in committed, monogamous relationships or practicing safe sex/abstinence shores up the false notion that gay sex is necessarily risky sex and that queer bodies pose a threat to the purity of the blood supply, which has already “reached a breaking point.”[10] This further suggests that such blood is not meant for queer people and especially not for HIV-positive individuals. The desperate need for blood after the Pulse shooting and the inability for gay men to alleviate this need for members of their own community thus seems particularly perverse for a community already struggling with limited resources and enduring social stigma.
In the Photo: Two men covered by a Gay Pride flag Photo Credit: The Telegraph
On Pulse’s website, owner Barbara Poma devotes a section to the nightclub’s history. Poma opened the club in 2004 after being inspired by her brother, John, who first introduced her to Fort Lauderdale’s gay nightlife scene. Poma ultimately named Pulse in memory of John after his death from AIDS-related complications in 1991. Pulse, as she says, was always meant to keep John’s heart beating. By animating John’s pulse through the club and its patrons, Poma keeps her brother’s and the Orlando queer community’s memory alive. The act of naming is powerfully symbolic: it connects the establishment to a long lineage of queer spaces that came generations before, as well as to the legacy of queer loss only decades before. The shooting at Pulse tragically reminds us that queer people disproportionately continue to face two epidemics: HIV/AIDS and the persistent risk of violence.
Recommended reading: “AFGHANS SILENT ON DEATH ON ORLANDO MASSACRE”
EDITOR’S NOTE: The opinions expressed here by Impakter.com columnists are their own, not those of Impakter.com.
Correction: [7/25/16] This piece has been corrected to express it is one of the deadliest mass shootings in history. Not the deadliest mass shooting in American history.
Further Reading:
[1] Treichler, Paula. “AIDS, Homophobia, and Biomedical Discourse: An Epidemic of Signification.” 43 (1987): 31 – 70. 32.
[5] For a brief but comprehensive legal take on the FDA’s policies since the 1983 ban on gay blood donation and its disconnect from medical advancements in the last two decades, see Bensing, Dwayne. “Science or Stigma: Potential Challenges to the FDA’s Ban on Gay Blood.” Journal of Constitutional Law. 14.2 (2011): 485 – 510.
[6] See Caplan, Arthur. “Blood Stains—Why an Absurd Policy Banning Gay Men as Blood Donors Has Not Been Changed.” The American Journal of Bioethics. 10.2 (2010): 1-2.
[7] Sontag, Susan. Illness as Metaphor and AIDS and its Metaphors. New York, NY: Picador. Original work published in 1989). 134.
[8] A term coined by cultural critic, Paula Treichler, to refer to the mass of shifting meanings that became attached to AIDS during the 80s and beyond.
[9] See Berkman, Winston and Li Zhou. “Ban the Ban: A Scientific and Cultural Analysis of the FDA’s Ban on Blood Donations from Men Who Have Sex with Men.” Columbia Medical Review. 1.1 (2015): 2-9 for a bioethical perspective on the discriminatory logics inherent in the FDA blood donation restrictions.
[10] Bensing 485.