What is Christmas like in Palestine at the time of COVID-19? There is no better place to find out about the challenges brought on by the COVID emergency than in Bethlehem, the birthplace of Jesus Christ. And in a hospital like the Holy Family Hospital run by the Order of Malta where most of the children in Bethlehem are born: It is both a center and a mirror of life in the region.
Until March 2020, life was normal in this sunny city of 25,000 people, six miles south of Jerusalem. Administered by the Palestinian Authority (PNA), people lived off tourism. And at Christmas, there was a peak of presence as pilgrims visited the Church of the Nativity, a UNESCO World Heritage site since 2012. In 2019, the Church was even removed from the UNESCO list of World Heritage Sites in Danger because it had been so well-restored. And people flocked there for Christmas, as always.
Not this year.
When COVID-19 hit, Bethlehem was the first city to go under curfew, closing hotels, tourist shops, and all economic activities. Later on, COVID-19 spread to the surrounding district and also to the other districts in Palestine. As most families in Bethlehem depend on tourism for their income, the pain was immediate and long-lasting.
The movement of people was drastically curtailed, except for medical personnel allowed to reach the medical centers. And I wondered how hospitals in the region addressed the COVID-19 emergency.
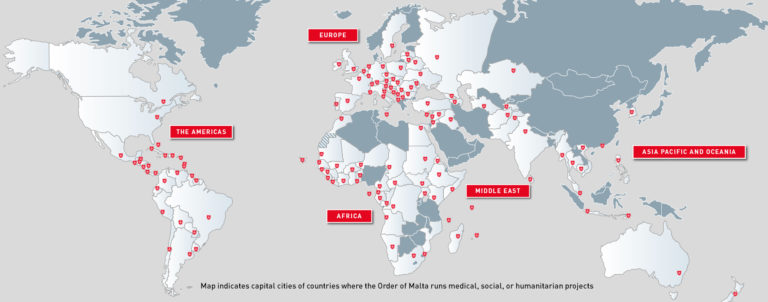
To find out, I contacted one of the hospitals on the frontline of the pandemic in Palestine, the Holy Family Hospital (HFH) run by the Sovereign Order of Malta, one of the world’s oldest caritative institutions. The Order is a lay religious order of the Catholic Church since 1113 and a subject of international law with permanent observer status at the United Nation. Over 135,000 people work for the Order, including 13,500 members and 42,000 professionals, mostly medical personnel, and the rest are permanent volunteers. The Order operates in 120 countries a broad range of medical, social, and humanitarian projects and activities:
The Holy Family Hospital in Bethlehem had been a general hospital for a century until it closed down in 1985. It was reopened by the Order of Malta as a maternity hospital in 1990 and today it has a staff of 172. It has accounted for over 88,000 deliveries since it reopened, delivering around 60% of babies in the region.
In 2019, 4626 deliveries were recorded, including 454 preemies. This year, the number of births is expected to be fewer, around 4,250.
Over the years, in addition to regular funding from the Order of Malta, HFH has received donations from the American Congress, the Belgian Government and the O’Neil Foundation that have permitted upgrading the facilities, including establishing a Diabetic Clinic for pregnant women, a Mobile Clinic to reach remote areas and, most importantly, a Neonatal Intensive Care Unit (NICU). The NICU, composed of 18 beds, is capable of caring for preemies at 24-weeks of gestational age. It is the only maternity hospital in the area that has that kind of facility.
Perhaps what is most remarkable about HFH is that, in line with the Order of Malta’s mission and mandate, it never discriminates: It is open to all patients regardless of economic and social status or religion and delivers babies from Christian, Muslim, and Jewish mothers alike. It also has a Poor Case Fund to provide additional financial support on top of the 50% medical subsidy that the Hospital provides to all patients.
The Poor Case Fund is playing an increasing role as the COVID emergency has destroyed tourism, the main source of income for most people. At present, almost half (45%) of the pregnant women come from a low socio-economic background with no kind of insurance coverage; 44% are refugee patients under the care of UNRWA and 2% are covered by the PNA; the remaining, just 9%, have a better economical status.
I talked to Ms. Elizabeth Anastas, the Hospital’s Director of Administration and Finance. Here is our conversation, abbreviated, and edited for clarity.
What happened when you first faced the COVID lockdown in March?
Elizabeth Anastas: From the beginning, we were in direct contact with the Ministry of Health to determine how to combat the virus under the current situation in Palestine. We always work closely with the Ministry of Health, as well as with other NGO-funded hospitals in Bethlehem.
Are you a referral center for the treatment of COVID19?
E.A.: We are not. But patients coming to the hospital know that they will receive the best medical care, especially when infected with COVID-19 which puts pregnant women and their babies at higher risk. This is where our intensive unit comes in and is so useful because for a patient with COVID 19 the risk increases and the need for a NICU is imperative. Also, HFH provides all needed obstetrics and gynecology services for COVID-19 patients who are not oxygen-dependent and do not need intensive care.
So what did you have to do to equip the Hospital to address the virus?
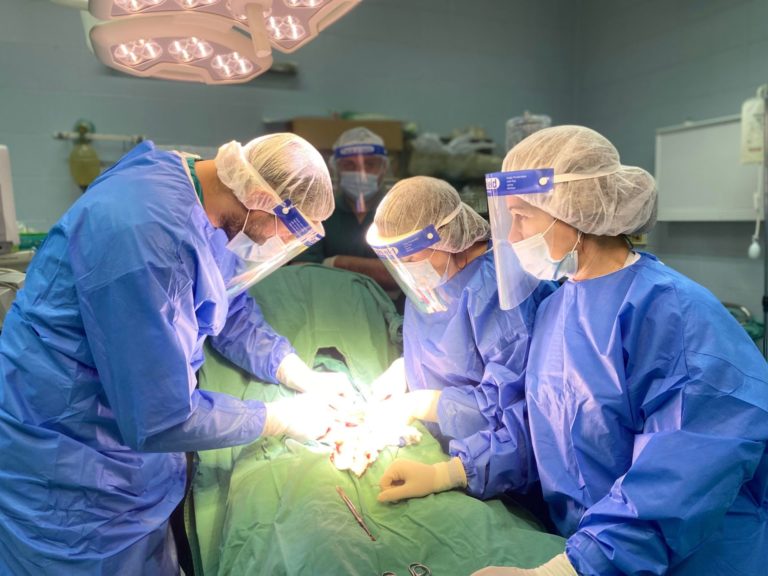
E.A.: Since the declaration of the State of Emergency on March 5th, we implemented an emergency plan to protect both our staff and the patients in order to maintain high-quality care provided for our patients. The emergency plan included several elements: The Staff was supplied with all the needed PPE’s in order to protect themselves and the patients; training was provided to the staff on using the PPE’s; special procedures were set up for dealing with suspected patients, including where and how to transfer infected patients, how to deliver an infected patient…etc.
In addition, a Triage room was established at the entrance of the hospital in order to examine every single person entering the hospital including the staff themselves. A special isolated room was also established in order to examine any patient coming with symptoms of infection. And that room was also equipped for an emergency delivery of any infected or suspected patient.

This was not simply a matter of adding equipment, it amounted to reorganizing the hospital structure. How did you manage?
E.A.: Well, the structure of the Hospital is a challenge since it is a building dating back to the year 1880. We were obliged to follow strict procedures since it is hard for us to completely separate the COVID area from the other patients.
A special dedicated Emergency COVID-19 committee was established that included the Supervisors of all the departments in the hospital in order to make sure that the information was reaching all employees correctly and at the right time. Most importantly, this ensured that all staff was made aware of the new protocols and guidelines that are updated every week in case anyone is infected. The goal is for every staff member to be able to provide high medical care safely and efficiently at all times.
How well did all your measures work out?
A.E.: Problems came not from us but from the lockdown itself. Many people were unable to reach our Hospital mainly those coming from Hebron and other villages surrounding Bethlehem. And that has translated into a loss of 30% in the number of deliveries compared to normal times. Moreover, the Ministry of Health closed down outpatient clinics for safety reasons; the lockdown lasted more than six months, hence, HFH lost the daily income generated from these consultations too.
Another factor external to the hospital was the loss of tourism: The whole region of Bethlehem suffered and family income was adversely affected. That had a knock-on effect, didn’t it?
A.E.: Certainly. People lost their income which affected their ability to pay for the services provided at the Hospital and this is imposing a bigger burden on our poor case fund that is limited. However, the door of Holy Family Hospital is always open without regard to whether patients are able to pay or not.
Adding to the problems is the rise in the cost of supplies and consumables due to the safety measures and more generally, rising prices during this pandemic.
Could you consider reducing staff in order to save money?
E.A.: The hospital is unable to reduce the number of staffing since the current number is highly needed especially during this pandemic. Our new Triage area at the entrance of the hospital is open 24/24 hours and needs at least 5 Midwives. Consider the complexity of the process: At the entrance (Triage Area) every patient entering the hospital has to respond to questions in order to detect whether there is a possible infection. The suspected or the infected patient is moved to the isolation room where she is examined by a dedicated doctor and Midwife.
In case the patient is in labor she is moved to a dedicated delivery room. The doctor and the Midwife stay with the same patient till the discharge after delivery in order to reduce the possibility of virus transmission and to limit the movement of the staff.
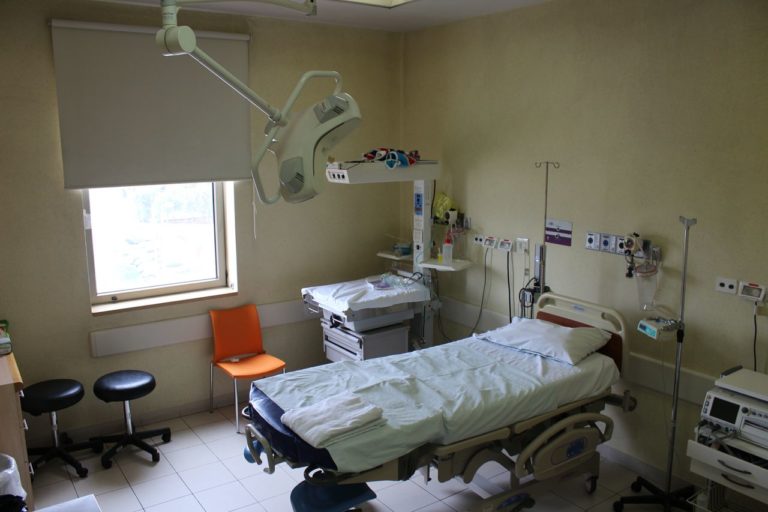
The infected mother and her newborn remain under the HFH supervision till the discharge and followed later on in the outpatient clinic.
Also, we have many staff absences as some are exposed to infected patients and had to quarantine, even if wearing needed PPE’s – but those are the rules imposed by the Ministry of Health. Or they got infected by a family member who was infected. Their absence had to be covered by the others in the team.
How many were infected by COVID-19 at the hospital since the emergency began?
E.A.: The total number of women with COVID19 who received medical care at our hospital since June is 23. While 26 Staff members were infected with COVID19.
Considering the measures you have to take to handle Covid cases, the impact is enormous. What other challenges did you have to face?
E.A.: I can think of many: Having the proper PPE’s was not easy as many times they were short in the Palestinian market; when a staff member is sick with Covid -19, providing them with the needed support so that they come back to work in good health; receiving pregnant women with positive covid-19 status, thus requiring us to follow special procedures; receiving pregnant women who are especially in need of medical therapy like oxygen-dependent patients who need ventilation, and the difficulties faced in transferring them to a general hospital.
More generally, there is a lack of oxygen generators in the Bethlehem district as a result of the recurrent malfunctioning of the oxygen generator in the national center of Covid 19 in Bethlehem. We are on the first line to help the center as we provide them with oxygen bottles filled on our premises.
You were busy before but with Covid, you are busier than ever. Thank you for taking the time to respond to my questions. I would like to add a link for anyone moved to make a donation, click here: Birth Place of Hope.