The Ethical Implications Of Health Professionals Refusing Treatment Due To Their Religious Beliefs.
In early September 2015, Kim Davis who is the elected Deputy Clerk of Rowan County in Kentucky was jailed for five days for not dispensing marriage licenses to gay couples. This occurrence has sparked great controversy and brings forward the thin line between religious belief and discriminatory conduct. The grey area that Ms. Davis has endeavored into is often touched upon in the field of medicine. Her decision not to dispense marriage certificates to gay couples is due to conscientious objection.
Conscientious objection is when a person is asked to perform an act that goes against their religious beliefs. This act can lead to a ripple reaction of consequences that can compound the problem; this is sometimes referred to as the slippery slope effect. Some practitioners cite conscientious objection when they refuse treatment to a patient due to religious beliefs. When the clinician refuses treatment the patient may experience an inability to get care, which will cause other problems, hence the slippery slope effect.
Ms. Davis is not in a profession that can physically harm a person due to her conscientious objection, but her actions may escalate others to follow her behavior. Healthcare providers do have the ability to indirectly harm a patient if a requested treatment is not given. They are professionally responsible to oversee the care of the patient. Ms. Davis’s actions are showing others with similar beliefs to forgo their professional duties and force others with differing beliefs to suffer. Her choices have the potential to perpetuate discriminative behavior and can have potentially dangerous consequences.
There are other states threatening to follow Ms. Davis’s actions due to their religious beliefs. In June 2015, the United States Federal Government passed a law that made gay marriages legal, which was met with heavy resistance from many southern states. Ms. Davis not only stopped dispensing licenses to gay couples, she instructed her colleagues (including her son who is also a clerk) not to provide licenses to the gay population. She is an Apostolic Christian since 2011 who believes a marriage is between a man and a woman. Although Ms. Davis is not Catholic, she even received a secret visit from Pope Francis to offer support for her plight.
How far will professionals take their religious beliefs in their quest to honor their God?
 In the Photo: Pharmacists have refused to distribute birth control due to conscientious objection.
In the Photo: Pharmacists have refused to distribute birth control due to conscientious objection.
As a federal employee, she is required to follow the law regardless of religious belief. Physicians take an oath that places patient care above all else. Unlike Ms. Davis, there are very little consequences for physicians citing conscientious objection. The only consequence is providing less than ideal care to the patient. Mrs. Davis is facing more prison time and large amounts of sanctions if she continues to refuse to fulfill her professional duties. How far will professionals take their religious beliefs in their quest to honor their God? Should Ms. Davis and clinicians be permitted to work in a position where their personal beliefs directly interfere with their professional duties?
The title of professional implies there is an ability to separate between personal and work related responsibilities.
Practitioners are faced with several ethically challenging cases that often leave them declaring conscientious objection. This decision to deny a patient treatment for any reason has the potential to have a slippery slope effect. If a pharmacist refuses to fill out a birth control script due to the abortive effects, the patient must find another pharmacist that is willing to give the medication. If this patient is unable to locate a pharmacy in a timely manner, she may be forced to forgo a dosage. By skipping the dosage, the patient will risk a potential pregnancy and for some women cause an imbalance of hormones that leads to mood swings and acne. There are some pediatricians who refuse to prescribe birth control to their young patients due to conscientious objection. Since the patient is under age, the parent must approve the usage of the pill.
………………………………………………………………………………………………………………….
Related Articles:“SAVING LIVES – THE MORNING AFTER PILL IMPACT” by ALESSIA MINICOZZI
“HOW CLIMATE CHANGE CONTRIBUTES TO THE GLOBAL PUBLIC HEALTH CRISES” by ANDREW BUDSOCK
………………………………………………………………………………………………………………….
Regardless of gaining approval from the parent, some pediatricians will force the parent to change doctors. This physician may have cared for the child since their birth. Due to the pediatrician’s religious beliefs, the parent and young patient are forced to rebuild the trust with their child’s new doctor. The relationship between a pediatrician and their young patient and parent takes some time to develop and preserve. Adolescents tend to have difficulty in sharing personal information, particularly when it relates to sexual activity. When the pediatrician has personal religious views that interfere with having an open and frank discussion about sex, the adolescent is less likely to make healthy decisions. Also, some pediatricians believe that prescribing birth control may encourage sexual activity before marriage. If the pediatrician refuses to prescribe birth control, the adolescent must wait to locate another practitioner that is willing to provide the medication. This waiting period may cause the adolescent to proceed with unprotected sex or deal with a number of health problems that the pill could have avoided. The parent may have to deal with a teenage pregnancy and unwarranted judgment from the practitioner.
There is a thin line between conscientious objection and discrimination.
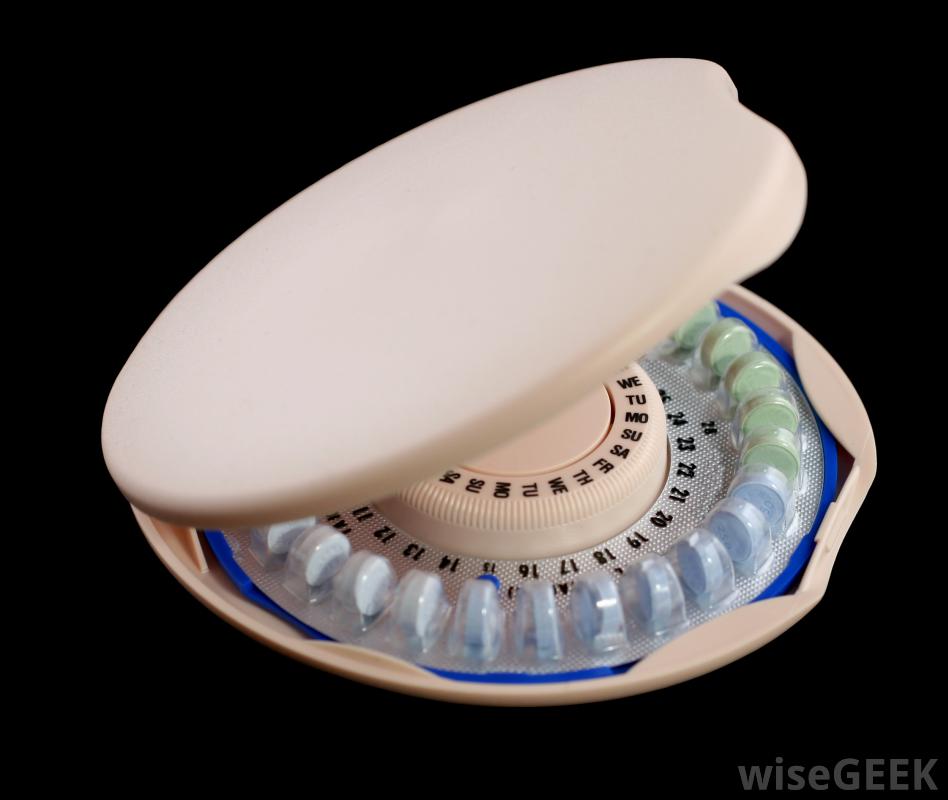 In the Photo: Some women have to go to multiple pharmacies in order to get her birth control. Source: WiseGEEK
In the Photo: Some women have to go to multiple pharmacies in order to get her birth control. Source: WiseGEEK
Some practitioners may be less obvious with their conscientious objective beliefs. A healthcare provider may want to defer a gay patient with HIV to another colleague. Some clinicians do not want to encourage same sex activity by providing safe sex information. The practitioner does not have to reveal the reasons for exchanging patients to another clinician. This exchange can take place in a discrete manner, never revealing the reason behind this decision. This time lapse in locating another physician willing to care for this patient may postpone treatment to the HIV patient by increasing their white cell count. The larger the white cell count, the greater the risk of the patient heading into AIDS.
This simple act of deferring the patient may seem relatively harmless, but there is a thin line between conscientious objection and discrimination.
As the cases become more complex in nature, conscientious objection becomes harder to fight against. In the field of palliative medicine there are circumstances where the physicians may prescribe a large amount of a sedative or pain medication that has the potential to accelerate the death of a terminally ill patient. Once again, the physician may refuse to write this script due to the possibility of causing passive euthanasia, unintentional early death, which is against some religions. If the patient does not receive this dose of medication, he could experience unbearable pain and stay in a constant agitated state.
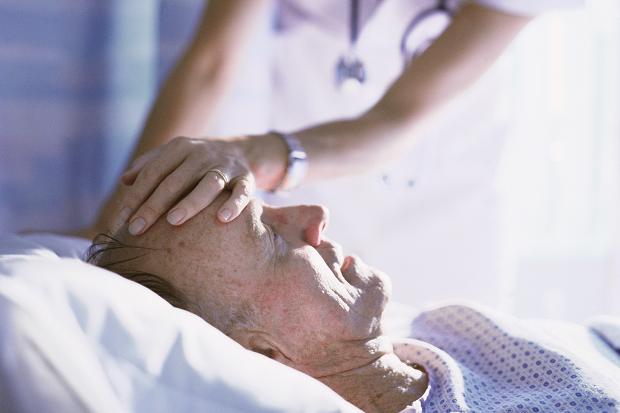 In the Photo: Caring for terminally ill patients is not so black and white.
In the Photo: Caring for terminally ill patients is not so black and white.
To maintain the patient in such an uncomfortable state, the patient’s loved ones may be left with a negative and harsh image of the dying process. Under similar circumstances, a pharmacist may be asked to fulfill an order of a large dosage of pain medication that may unintentionally kill the patient. Many terminally ill patients are left in agony due to the pharmacist refusing to dispense the medication. Some terminally ill patients build a tolerance to pain and sedative medications, which require the dosage to increase in order for it to be effective. When the pharmacist refuses to provide the prescribed medication, it is in direct violation of their professional duties. A pharmacist is suppose to safeguard the prescriber, not to make decisions regarding the level of dosage the patient should receive.
Once medical practitioners start to stray outside their professional duties, then accountability goes amuck. Should a health care provider continue to practice medicine when they will occasionally face issues that cause them to cite conscientious objection?
Healthcare providers are met with countless patients that will question their conscience. They are forced to make decisions that may challenge how they treat patients. When a healthcare provider refuses to fulfill their professional duties, the patient at the very least is inconvenienced, in the extreme directly harmed. Although there are parameters in place when a practitioner is faced with a conscientious objection case, deferring the patient to another colleague can have a slippery slope effect. This handing off of the patient to another colleague can be concerning. There is no way to assure follow up with the patient to see if she received the proper care. This referral may be outside the patient’s health insurance network or far in distance to where the patient lives. The patient may have built a bond with his practitioner and may feel betrayed or judged by their referral. A patient who has a long-standing relationship with her OBGYN who refuses to perform an abortion can see this as a betrayal and judgment. This patient is use to sharing her medical history with her OBGYN and now is forced to find an unknown practitioner that is willing to perform the procedure.
How inconvenient should the patient be to accommodate his healthcare provider’s religious beliefs? In the end, should professionals be permitted to continue to practice in a field they cannot fulfill their duties? Does conscientious objection trump the role of providing exceptional care to patients? These are questions that may not be answered today, but will likely be relevant for many decades to come.









