As the ubiquity and reality of climate change beckons the international community into action, tangible consequences are appearing ever more pervasive. With COP21 quickly approaching, it is important to highlight the effects of climate change to both human and natural spaces, while also recognizing how the two overlap. In addition to climate change putting food systems at risk and food security becoming a larger issue, public health is also being negatively impacted through the effects of climate change.
Currently, some 750 million people are at risk of food borne trematode disease, or 10% of the global population. This striking statistic has brought food borne trematode illness to the forefront of public health research and sustainable development initiatives. Unfortunately, these illnesses are linked to socio-economic status and poverty. Therefore, populations most at risk are those living in developing nations, particularly in rural areas with limited infrastructures. Many trematode diseases are food- and waterborne; it is therefore essential to understand the the ecological dynamics of the areas of infection along with identifying the appropriate environmental policy. This requires a bottom-up approach, relying on regional health initiatives that are sensitive to local cultural needs and inclusive to all stakeholders.
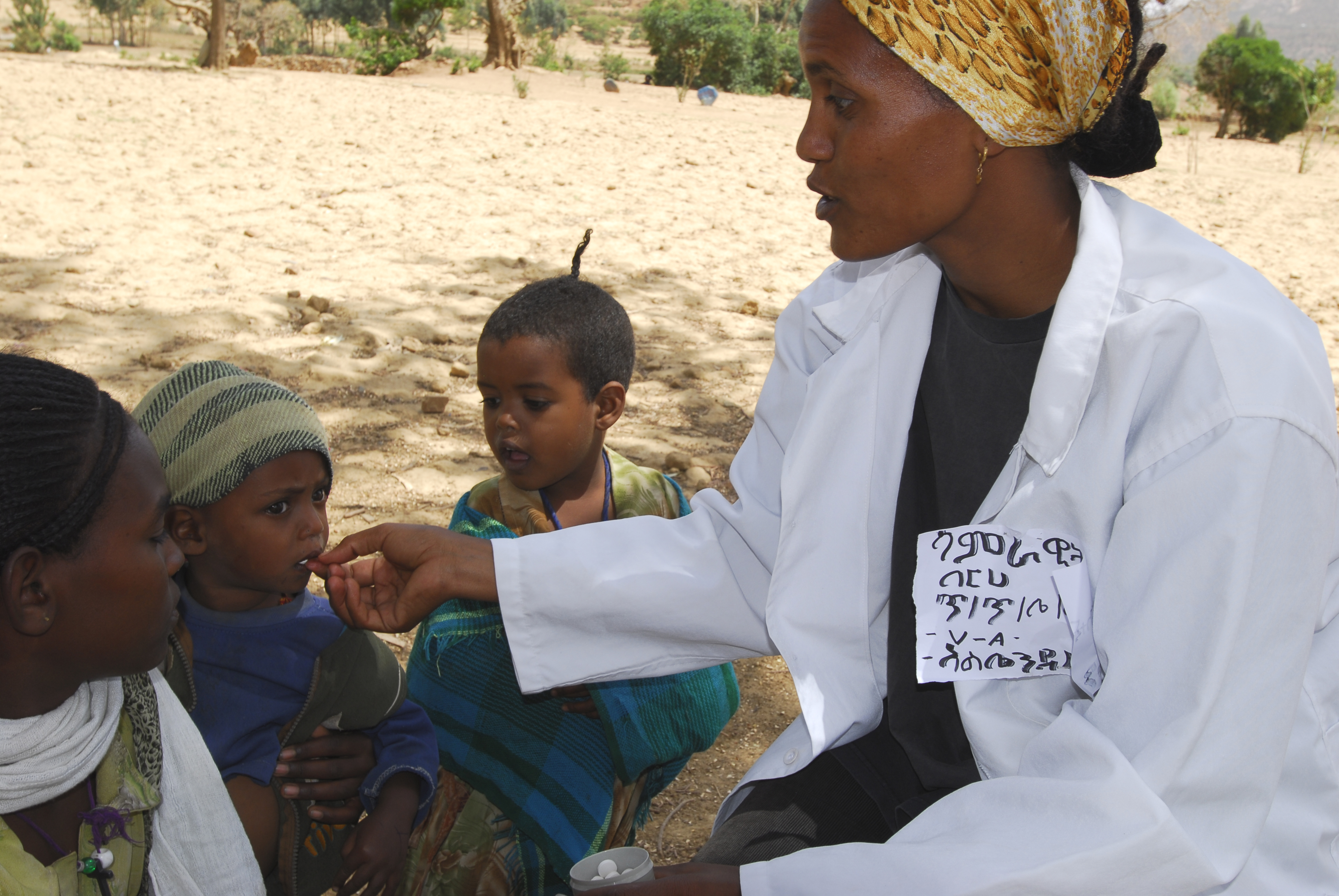
In the photo: Health extension worker gives a child deworming tablets in Endaba Gerima Sub-district, Tigray Region, Ethiopia– photo credit to UNICEF Ethiopia
Two prominent food borne trematode illnesses are Opisthorchis viverrini, (O.v.) and Schistosomiasis. Both are exceedingly difficult to pronounce and serious health threats, particularly in Southeast Asia, including southern China, and eastern Africa. Individuals become infected by O.v. by consuming raw fish, while for Schistosomiasis, people are infected by coming in contact with contaminated water. For both illnesses, poor waste treatment facilities contaminate local water resources, so the feces from infected individuals is reintroduced into their water systems. Treatment for both illnesses involves a drug called Praziquantel; however, people can still become reinfected after treatment, and cost and access to the drug can be a challenge for some communities.
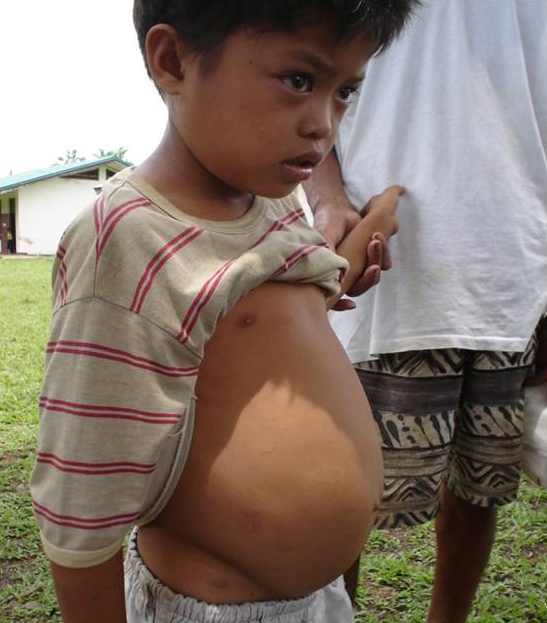
In the photo: A young boy in Agusan del Sur, Philippines suffers from a build of of fluid in his peritoneal cavity, one of the symptoms of Schistosomiasis – photo credit to SuSanA Secretariat
Symptoms of O. v. and Schistosomiasis are mild with slight abdominal pain, discomfort, and diarrhea. For O.v., however, it can become more complicated. The International Agency for Research on Cancer, IARC, classifies O. v. as a Group 1 Carcinogen because of the strong correlation between prolonged exposure to O. v. and incidence of cholangiocarcinoma (CCA), or cancer of bile ducts which drain bile from the liver into the small intestine. CCA is responsible for 19% of liver cancers in the United States, compared with 71% in the Province of Khon Kaen, Thailand, where prevalence of O.v. can reach up to 71%, representing the highest incidence of CCA in the world.
The World Health Organization has both illnesses on the list of Neglected Tropical Diseases (NTD). As a result, there has been an increase in investments to fund research for better treatments and prevention. Specifically, the Schistosomiasis Vaccine Initiative is a collaboration between the Sabine Vaccine Institute, George Washington University, the Oswaldo Cruz Foundation, the Chinese Institute of Parasitic Diseases, the Queensland Institute of Medical Research, and the London School of Hygiene and Tropical Medicine and aims to develop a vaccine for Schistosomiasis. In January 2015, Phase 1 clinical trials began for the Sm-TSP-2 Schistosomiasis vaccine, so what was only hope for systematic prevention is fast becoming a reality.
In an economic context, finding solutions for NTD shouldbe viewed as solid investments. The World Health Organization suggests that if we can achieve the 2020 targets for the 10 most debilitating NTDs, healthier citizens would generate an estimated US$623 billion in increased productivity between 2015 and 2030.
In the photo: Severe flooding in Thailand in 2011 leaves communities underwater and at greater risk of O.v infection – photo credit to dany13
However, climate change may be undermining efforts to mitigate the prevalence of these diseases.
Ample evidence suggests that climate change could have a significant impact on the spread of both diseases by changing rainfall patterns and intensity, consequently providing environments for both O.v. and Schistosomiasis in which they persist. The latest report (AR5) from the Intergovernmental Panel on Climate Change (IPCC) states that climate change may increase drought and rainfall intensity. This means there could be fewer rainy days, but more extreme weather events, so the hard-dry surfaces create a pooling effect when it rains because the water has nowhere to go. This may increase flooding in the region while also mixing contaminated water and bringing it to previously uninfected areas. In addition, flooding may stress already weak waste treatment facilities, which would only further contaminate water supplies. This highlights a reoccurring issue for sustainable development projects, which is that initiatives for education and training may not be enough to get over the infrastructure hurdle that is being ever more challenged by climate change.
Cultural issues add another layer of difficulty to Ov.
Various media reports and prevention initiatives have suggested that ceasing the consumption of raw fish is the perfect solution to the problem. However, this fails to capture the whole story, and highlights a top-down mentality that doesn’t translate well for sustainable development. The Isaan people of Northeastern Thailand are an ethnic minority and have had a tumultuous relationship with the Thai government for decades. Food is an important part of any culture, and for the Isaan people this food is raw fish, specifically a dish called Koi Pla. Consequently, the Thai government instructing the Isaan people to stop eating Koi Pla would only further alienate this minority group. This compounds the issue of Ov, but a clear focus on inclusive bottom-up workshops and educational seminars may help get the message across in a more nonthreatening way.
In the photo: Thai fishermen catches fish in nets, including potentially infected ones, to prepare raw fish-based meals, such as Koi Pla – photo credit to Banchob Sripa et al. 2007 in PLoS Medicine
Public health issues are global, percolating into all cultures and compounded by climate change. This highlights the need for a collaborative interdisciplinary approach to developing solutions.
Fortunately, many of these environmental health issues are covered in the new 17 Sustainability Development Goals (SDGs) just adopted by the United Nations General Assembly. The call for a healthy, sustainable, and equal world has never been clearer, but these goals are only a framework to organize efforts on the ground. Therefore, the key to achieving the new SDGs is an inclusive and bottom-up approach that gives communities a voice as well as the necessary funding to make it a reality. However, to empower and mobilize people to innovate and enact change, we first need to get them healthy.