This may come as a surprise to most people: The numbers show that Africa has a COVID-19 plan to address the pandemic that (for now) is working. Consider the situation.
First, let’s take a look at how Africa has fared in terms of deaths caused by COVID-19 compared to similar-sized geopolitical units: Europe writ large includes 50 very small and large countries; the United States with 50 separate States; and the African Continent with more than 50 countries. All three have roughly the same number of geopolitical jurisdictions.
Here are the number of reported COVID-19 deaths between them (as of 15 October):
Africa: 38 830 deaths; the five countries reporting most deaths are South Africa (18 151), Egypt (6 077), Morocco (2 726), Algeria (1 827) and Ethiopia (1 312).
America: 600 543 deaths; the five countries reporting most deaths are United States (216 872), Brazil (151 747), Mexico (84 898), Peru (33 512) and Colombia (28 306).
Europe: 236 437 deaths; the five countries reporting most deaths are United Kingdom (43 155), Italy (36 289), Spain (33 413), France (33 037) and Russia (23 205).
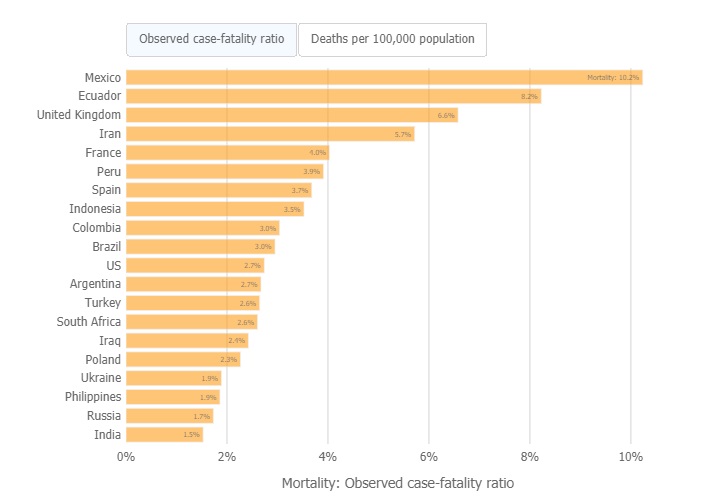
In terms of populations, the African Continent is by far the largest with over 1.2 billion people and it has had over 1.6 million cases. South Africa is the only country on the entire continent among the 20 countries with the highest deaths per capita, and even among those, South Africa is among the lowest with roughly 696 000 cases.
The chart above, updated on 15 October 2020, shows the number of deaths either per 100 confirmed cases (observed case-fatality ratio) or per 100,000 population (this represents a country’s general population, with both confirmed cases and healthy people). Countries at the top of this figure have the most deaths proportionally to their COVID-19 cases or population, not necessarily the most deaths overall. Source: Johns Hopkins
Numbers are deceptive and often misleading, and antibody testing is likely to show many more infections and data from many African countries. Such information has been suspect in the past. Indeed, skeptics will point out Africa’s COVID-19 performance looks good “on paper” but starts with a much younger and less urbanized population, insufficient data collection capability, and a history of poor execution without extensive outside help.
While there is reason to be skeptical, other places and people should not throw sand or stones, especially when Africa has a more coherent approach to COVID-19 than either the United States or the European Union.
The Context: A Rising Population, Conflicts, Weak Structures, Recurrent Pandemics (like Ebola)
Over the last decade, in Africa the probability of a pandemic has risen and expected to continue. Many factors contribute to this situation: weak national health systems, high population growth rates, conflict and state fragility, rapid urbanization, the large-scale movement of people, goods and livestock across borders, the adverse effects of climate change, and the dense proximity of animals and humans. All these factors drive the emergence and re-emergence of infectious diseases.
Rates of communicable disease morbidity and mortality remain stubbornly high on the continent. And the rising risk of pandemics threatens hard-won gains in social and economic development throughout the region.
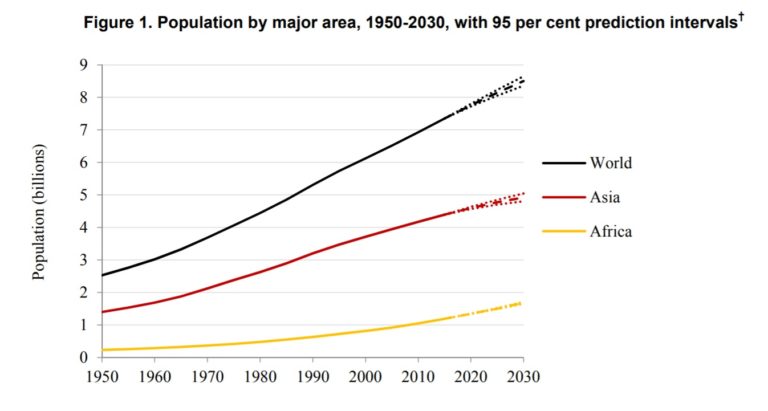
Nearly two-thirds of the population is under 25 years old, with the continent’s total population increasing by about 30 million people each year. The United Nations projects that the African population will reach 1.68 billion by the end of the next decade, an increase of 500 million people between 2016 and 2030:
 The 2014-2015 West Africa Ebola outbreak infected more than 28,000 people and killed an estimated 11,000. Despite its relatively difficult transmission mechanism, Ebola devastated national health systems, disrupted regional economies, inflicted lasting reputational damage that discouraged travel and investment, and revealed systemic vulnerabilities in Africa’s infrastructure.
The 2014-2015 West Africa Ebola outbreak infected more than 28,000 people and killed an estimated 11,000. Despite its relatively difficult transmission mechanism, Ebola devastated national health systems, disrupted regional economies, inflicted lasting reputational damage that discouraged travel and investment, and revealed systemic vulnerabilities in Africa’s infrastructure.
In West Africa where Ebola ran rampant in those years, virtually all countries of the West Africa Health Organization have now put in place regional disease surveillance system enhancement approaches. Launched in 2016, the Regional Disease Surveillance Systems Enhancement (REDISSE) Program was largely financed by the World Bank. The financial arrangement is complex, using a combination of the World Bank’s International Development Association (IDA) credits and grants, International Bank for Reconstruction and Development (IBRD) loans ($60 million for Angola), and multi and single-donor trust funds.
REDISSE involves 16 African countries in the sub-region and works on three fronts:
- addressing weaknesses in human and animal health systems for disease surveillance and response;
- building capacity for effective cross-sectoral and cross-border collaboration; and
- providing an immediate and effective response to emergencies.
By 2019, REDISSE had built up a local capacity to respond to the challenge of diseases and help protect countries from epidemic threats due not only to Ebola but – and this is important – also resulting from other pathogens such as COVID-19.
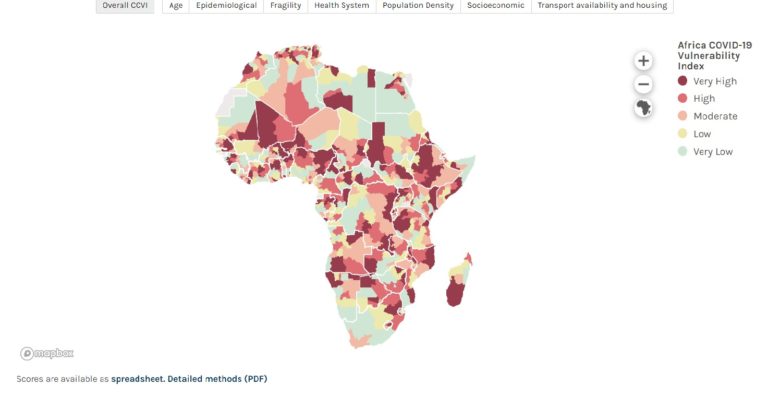
A useful window on the Africa situation at the sub-national level and future prospects is provided by the Africa COVID-19 Community Vulnerability Index (CCVI). Produced by the Surgo Foundation (with support from DFID, the United Kingdom’s official aid agency), it is the first Pan-African in-depth index of vulnerability to COVID-19.
The Africa CCVI (screenshot is shown above) ranks 751 sub-regions across 48 African countries in terms of vulnerability to COVID-19 based on seven key themes: socioeconomic status, population density, access to transportation and housing, epidemiological factors, health system factors, fragility, and age of the population. The dashboard is interactive: By clicking on various regions of the map, details relating to all these factors show up and are ranked in relation to other regions – the darker the shade on the map, the greater the vulnerability, and blue indicates very low vulnerability.
Sema Sgaier, the Surgo Foundation Director put her assessment this way:
“I look at Africa and I look at the U.S., and I’m more optimistic about Africa, to be honest, because of the leadership there and doing their best despite limited resources.”
In fact, it is possible now to directly confront the situation in Africa by comparing the Africa CCVI with the American COVID-19 Pandemic Vulnerability Index (PVI) Dashboard after which it is modeled. These CCVIs were developed through a collaborative effort by scientists from the National Institute of Environmental Health Sciences (NIEHS), North Carolina State University and Texas A&M University.
Leadership: The Birth of the Africa CDC
America presented Africa with another model, its famed Centers for Disease Control and Prevention with an unimpeachable reputation, having in particular recently played a major role in the fight to overcome Ebola. African leadership rose to the challenge. In 2017, the African Union, composed of 55 countries, created the Africa Centers for Disease Control and Prevention (Africa CDC) and committed 5% of its operating revenue to support this new institution.
The Africa CDC attracted multiple international financing, including from the U.S., China, the European Union, international financial institutions, and a range of other donors as well as technical assistance from major international institutions, including WHO, the World Organization for Animal Health, FAO, CDCs from China, the European Union, and the United States, among many others. All this provided the wherewithal to perform an ambitious mandate.
John Nkengasong was appointed to be the Director of the Africa CDC. He has brilliantly steered its member countries into an alliance praised as responding better than many richer regions and countries. Nkengasong is a Cameroon-born virologist who was formerly with the U.S. Centers for Disease Control and Prevention. Recently he was awarded the Gates Foundation Global Goalkeeper Award as a “relentless proponent of global collaboration”.
The Key Role of Africa CDC: Laboratory Network Coordination, Testing, Medical Supplies Procurement, Research, Safety Monitoring and the One Health Approach
The list of critical actions taken or in the works represents an incredible and far-reaching effort. A veritable “united and continental strategy”.
The Africa CDC rolled out in less than three years an impressive series of related and complementary structures:
- the Partnership to Accelerate COVID-19 Testing (PACT): Test, Trace, Treat to strengthen covid testing capacity and test at least ten million Africans over the next six months;
- the Africa Medical Supplies Platform, in partnership with the African Export-Import Bank, to facilitate country procurement of critical medical and laboratory supplies from certified suppliers;
- the Pathogen Genomics Intelligence Institute connecting research centers conducting genomic sequencing with public health institutes and removes potential silos between national initiatives while the continent faces a singular disease threat;
- the “Regional Integrated Surveillance and Laboratory Network” (RISLNET) that coordinates and integrates public health laboratory, surveillance, and emergency response assets, including public health data, at the regional level to effectively support prevention, rapid detection and response to current and emerging public health threats within defined geographic regions of Africa.
Most importantly, Africa CDC incorporates the One Health approach –the interactions between animal-human-environmental aspects into many aspects of its regional work. This includes assessing the capacity of human and animal health laboratories in Africa and financing BSL-3 laboratories for accurate diagnosis of infectious diseases and antimicrobial resistance.
Africa CDC is piloting an innovative “One Health” approach at the regional level to adopt a “holistic, health in all policies” to address emerging and re-emerging zoonotic infections. Further, it is developing guidance for National Public Health Institutes to incorporate zoonotic diseases and One Health activities into their surveillance, emergency preparedness, workforce development, and disease control programs
These achievements are remarkable for Africa and in particular the Africa CDC, given its three-year existence.
Certainly, Africa faces fragile health systems, limited funding, recurrent disease outbreaks with late detection, economic challenges, and political turmoil. But so far, it is outperforming many other regions and countries. Hats off to Africa and maybe others can study and learn.
Editor’s Note: The opinions expressed here by Impakter.com columnists are their own, not those of Impakter.com. — In the Featured Photo: Africa CDC announces the launch of the Africa Pathogen Genomics Initiative (Africa PGI) with a US$100 million four-year partnership to expand access to next-generation genomic sequencing tools and expertise; Africa PGI will be part of the Institute of Pathogen Genomics, launched by Africa CDC in 2019. Source: Africa CDC