“Mom, Dad I want to become a physician.” Most parents hearing this sentence from their college student are extremely excited and proud. Some may naturally feel overwhelmed with the prospect of hundreds and thousands of dollars in medical school tuition bills, but most would gladly undertake this burden in order to say my son or daughter will be a doctor. The status of sporting a medical degree in the United States is the pinnacle of professional success. Physicians are well esteemed and revered in almost any situation. When there is an emergency in a public place, the first thing that is yelled “Is there a doctor here?” Doctors have the skill set to save lives and for this alone they are seen as superheroes. This constant call on their services means that physicians can never put themselves on the back burner.
Doctors rarely know when to ask for help when they feel burnout and overwhelmed. Physicians are always on the “go” and never know when to press, “stop.” Rather than feeling pride and blindly embracing the college student’s decision to become a doctor, the parent should consider the unique challenges that come with this career choice.
For some families, the feeling of pride for their child wanting to become a doctor quickly turns into a nightmare. When Kevin Dietl told his parents that he wanted to enter the field of medicine, the Dietl family was thrilled to have a son as a prospective doctor. They felt that as parents having a son that wanted to enter a profession as esteemed as medicine was ideal. However, they slowly saw their son withdraw from the family and turn into someone they did not recognize. On April 23, 2015, weeks from earning his medical degree, Kevin committed suicide. Nearly two years to the date before Kevin’s death on April 12, 2013, a third year medical student named Kaitlyn Elkins committed suicide. A year later, unable to deal with her daughter’s death, on August 29, 2014, Kaitlyn’s mother decided to take her own life. Kevin Dietl’s mother was convinced that if Kevin had access to support and resources that did not stigmatize voicing distress, her son would still be alive.
The changes that need to take place within the field of medicine in order to improve the quality of life for physicians are slow moving.
Asking for help as a medical student is sometimes seen as a sign of weakness. Some senior physicians in a teaching position are more inclined to react to the student’s need for support by either embarrassing them or making it impossible to ask for assistance again. The medical community turns a blind eye to the strain fellow physicians are under. If they were able to withstand the same strain when they were training, they reason, why should they lend a hand to junior doctors?
Little research is available that shows patterns of behavior that would provide reasoning for these suicidal tendencies. Some evidence indicates that male physicians are slightly more inclined to commit suicide than female physicians. What seems to be a consensus among the families of the suicide victims and some practicing doctors is a need for a major overhaul in how physicians are trained.
The changes that need to take place within the field of medicine in order to improve the quality of life for physicians are slow moving. The training process has not altered significantly for nearly a century. Only recently has the framework and cultural belief system made minor advancements. A doctor must still proceed through premedical school courses, achieve a high score on the MCAT, complete medical school, match at a residency program, and if this individual wants to specialize in a field of medicine, proceed through a fellowship in order to be labeled a doctor. The training process can last anywhere from 11 to 15 years. This arduous rite-of-passage has lead certain trainees and professionals to burnout and in some extreme circumstances commit suicide.
During this time, students, residents and physicians are expected to go without sleep, endure extremely limited social interaction, witness endless tragic medical cases, and withstand ridicule from senior doctors. This ridicule from senior doctors is often compared to military hazing. This hazing process is sometimes referred to as “pimping”. Pimping is when a senior physician puts a junior physician on the spot with a medical question. This process is to teach the junior physician how to think under pressure. If the junior physician does not provide the correct answer, the senior physician may feel the need to humiliate the junior physician in order to make an example out of him or her.
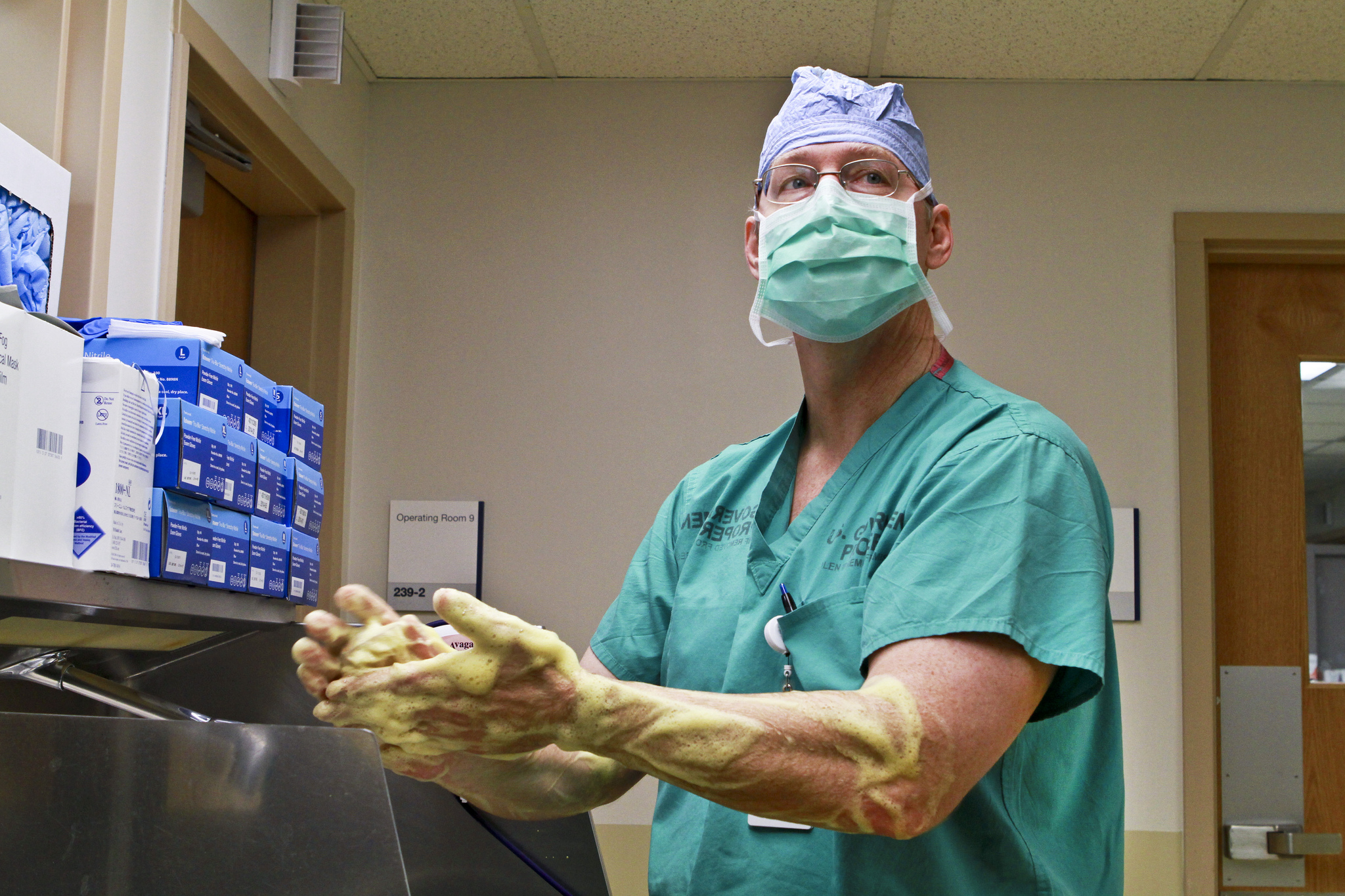
In the Photo: A doctor scrubs in for surgery. Photo Credit: Army Medicine
By performing this archaic exercise, the senior physician gets a sense of superiority, thus perpetuating the act of pimping. Pimping is a form of bullying. When junior doctors witness their colleagues get mistreated, they are less inclined to reach out for support. Furthermore, locating a senior doctor that will confront a fellow senior physician is rare. There are limited resources for junior physicians to rely on when they feel ridiculed or angry. Being mistreated in medicine is not an unusual occurrence. It is up to the medical professional to develop the coping mechanism to deal with the stress of bullying and negative behavior. Physicians are forced to witness tragic and overwhelmingly complex medical events that take place at work. It is expected that doctors do not demonstrate the effects of being bullied or show emotion.
Related Articles: “WOMEN MAKING THEIR OWN FERTILITY DECISIONS” by SHEENA DASANI
“THE SLIPPERY SLOPE OF CONSCIENTIOUS OBJECTION” by ALESSIA MINICOZZI
Pimping and the suppression of emotions are not the only negative aspects of medical training or practice. As a resident, there is a requirement to stay awake for nearly 36 hours. In certain states, there is a law to limit the amount of hours a resident is allowed to stay awake. The Libby Zion Law was past in 1989 in New York, which was commissioned by the Bell Commission Report. This law does not allow residents to work more than 80 hours a week and an attendent has to be present at all times.
It all started with the Libby Zion case. She was brought to the Emergency Department in 1984 and later that night admitted to the hospital. She presented a series of unrelated symptoms, but she was never given a drug toxicology test. The first year resident, known as an intern, who was awake for more than 36 hours reluctantly called his senior resident while he was sleeping in the residency quarters. Within several hours, Libby was given many medications that may have interfered with a drug that she took at home, thus leading to her death. Libby’s father was an attorney and a journalist at the New York Times and decided not to allow his daughter’s death go unresolved.
Mr. Zion turned his daughter’s death into a campaign to improve the working conditions of physicians-in-training. He was outraged by the number of hours the residents were forced to endure and make such serious medical decisions. He believed that fatigue was partially the cause of Libby’s death. Not only did Libby Zion change the amount of time physicians are allowed to stay awake, but it also demonstrated the culture of what takes place behind close doors at the hospital.

In the Photo: Endless hours of being on call leads to a useless doctor. Photo Credit: Flickr
The intern on call at the time of Libby’s death was reluctant to contact his senior resident because he was sleeping and was told unless it is urgent, do not contact him. Some senior residents and physicians do not want to be bothered due to their limited opportunities to rest, unless the junior resident is really in a compromised situation. This lack of supervision has led to many close calls and dangerous learning curves. Some senior physicians believe this is the only way to teach problem-solving and build skills that are helpful in an emergency. Once again, reaching out for help is a no, no amongst physicians.
This inability to ask for help when a physician is in distress is an ongoing issue throughout the duration of his or her career. There is a misconception that once physicians have completed the official training process, they have acquired all the coping skills needed to continue practicing medicine. In 2015, a photo taken by paramedics from California of an emergency physician went viral when he broke down after the death of a seemingly healthy 19-year-old patient under his care. After telling her parents, the doctor had to excuse himself to compose his emotions. As this photo went viral, the main focus was the physician’s human reaction to another being dying. He was not the doctor that lost his professional composure, but a man who had to tell parents that their daughter unexpectedly died.
If a doctor actively seeks assistance for their burnout they may face disciplinary action that can affect their medical license, lead to loss of hospital privileges, and result in inability for career advancement.
In this case, we have a doctor allowing himself to feel and not worry about what was expected of him as a physician. He knew enough to grieve a loss and return to patient care when he was ready. He clearly acquired the natural skills to avoid the all too common occurrence of burnout. There are a few studies that show if the physician is experiencing burnout there is a likelihood of suicidal thoughts. How was this emergency doctor able to find the strength to deal with the stresses of the job, while Kevin and Kaitlyn were not? There is never a definitive way to predict who will be affected by what occurs while practicing medicine. Due to these unpredictable coping abilities, it is advisable to have supportive resources in place for whenever physicians need help.

Viral photo of E.R. physician in California
Suicide and burnout among medical professionals rose steadily throughout the last decade. Doctors committed suicide at a rate more than twice the national average. Approximately, 400 physicians commit suicide every year. There is little data and statistics that explain the rise of suicide within this profession. One does wonder if the shame and to some extent denial of the medical community is the reason for the lack of hard data.
What is clear and evident is that more medical professionals are experiencing burnout and committing suicide as the years pass. This rise in burnout and suicide is cause for concern for certain medical professionals that have created campaigns and lectures. A family physician in Oregon is a self-proclaimed advocate for the prevention of burnout and suicide. There are also a few physicians that have left the practice of medicine in order to dedicate their time in providing a safe place for practicing physicians to avoid burnout and suicide. The aforementioned physicians are viewed as outliers at best and traitors at worst in their field. These emotions are sometimes used against them in a discriminatory manner. If a doctor actively seeks assistance for their burnout they may face disciplinary action endangering their medical license, leading to loss of hospital privileges and the inability for career advancement.
It takes a very resilient and unique individual to withstand the challenges of becoming a physician. This individual prior to entering the world of medicine should carefully consider all the obstacles they will be facing. No one should become a doctor without being fully informed and take the time to reflect. An individual entering medicine needs to learn to fight against the norm and never be afraid to ask for help. The idea that anyone inherently has the coping skills to proceed through the medical training process is absurd.
In order to develop well-rounded practicing abilities, the physician must feel safe to ask the tough questions and not worry about being criticized or bullied. Once the physician completes the training process the notion that doctors no longer require support and guidance is unrealistic. Medicine is a field that is emotionally filled with traumatic events and senior physicians will continue to face these occurrences throughout their career. There is never a time when physicians will not need some level of support. This reality is relevant and necessary to accept. Until medical administrators, fellow doctors, and educators realize that drastic changes are necessary to save physicians’ lives, the level of burnout will increase and the rate of suicide will accelerate.











