While the world and much of the medical and scientific community focus on dealing with COVID using effective vaccines and medications, other virus killers lurk in hiding which can become epidemics or pandemics, many emerging from the interface of the human/animal/ecosystem, One Health.
The Nipah Virus is just such a threat: It has the potential to cause widespread disease with a variety of symptoms and a shockingly high death rate of 40% up to 75%. But the good news is that a new vaccine is being evaluated which could prevent another pandemic similar to COVID or the earlier Ebola virus, both of which unexpectedly emerged and infected huge numbers of people.
Such outbreaks underscore the need to be ready to identify and then respond to an infectious outbreak that could morph into an epidemic–or worse. Indeed, scientists are now searching for universal vaccines which could break the cycle of catch up “at a minimum would be a shot that would stop a future pandemic, protecting against a yet-unknown coronavirus that will jump from animals into people in the years to come”.
As the Washington Post reports, vaccine scientists have been chasing variants; now, they’re seeking a universal coronavirus vaccine.
Prevention is worth pounds of response and having a viable vaccine in our arsenal which can be quickly brought to bear is smart preparedness and prevention. It is the latter which we have paid less attention to and need to do much more. Professor Aaron Bernstein, of the Center for Climate, Health and the Global Environment, Harvard University, rightly pointed out:
“Our salvation comes cheap [because] prevention is much cheaper than cures. […] If Covid-19 taught us anything, it is that we absolutely cannot rely on post-spillover strategies alone to protect us. Spending only five cents on the dollar can help prevent the next tsunami of lives lost to pandemics by stopping the wave from ever emerging, instead of paying trillions to pick up the pieces.”
The Challenges
Trying to develop a vaccine for any infectious disease is a monumental undertaking, costly in terms of human and financial resources, with the likelihood of success always a longshot; for example, there is still no effective HIV/AIDS vaccine after decades of trying.
A private pharmaceutical company has to consider the likelihood of its research investment producing a new marketable vaccine. It usually takes a very long time before a viable prototype is developed, sometimes years; then the company will need to run the gamut of a series of trials to get approval, and after all that, gauge how likely they will recoup their investment and generate profits.
This becomes even more dicey when most of the beneficiaries are in low-income countries and poor, and there is a likelihood of pressure from the global community to provide the vaccine at low cost – as was the case with HIV/AIDS medications. This is not an insignificant factor to be taken into the business decision equation.
Like HIV/AIDS, COVID “affects the rich as well as the poor.” From the outset, there were enough countries and consumers who could afford to pay, and it, therefore, attracted and accelerated huge research and investment commitments. Indeed, COVID triggered an all-out global effort to develop and bring to market multiple vaccine choices. Fortunately, this has been a great success saving millions of lives.
How Did We Get Here?
The real history of “Vaccines” began over 300 years ago when Lady Mary Wortley Montagu introduced smallpox inoculation to Western medicine after witnessing it during her stay in the Ottoman Empire.
While in the Ottoman Empire she visited women in their segregated zenanas, a house for Muslims and Hindus, making friends and learning about Turkish customs. There, in 1717, she witnessed the practice of inoculation against smallpox – variolation – which she called engrafting, and wrote home about it in a number of her letters.
Some 60 years later an English farmer, Benjamin Jesty, in 1774 saw that one of his dairymaids did not get smallpox (which was then decimating communities), despite having been infected earlier with cowpox. Jesty took his wife’s knitting needle (an “instrument” rarely mentioned), scraped pus from one of his cows infected with cowpox.
He next intentionally injected his son with smallpox using the knitting needle with cow pus, and the result was the boy showed no signs of infection. And in 1776, Dr. Edward Jenner did what neither of the earlier two had done, he used scientific methods, published his results, and is known worldwide.
This approach became “vaccination” (the origin comes from “vaccinia” or cowpox) and launched the birth of the science of vaccinology. Since then, many diseases have benefitted from vaccines and are given routinely worldwide. Polio, tetanus, influenza, rubella, measles vaccines have saved countless lives, especially children.
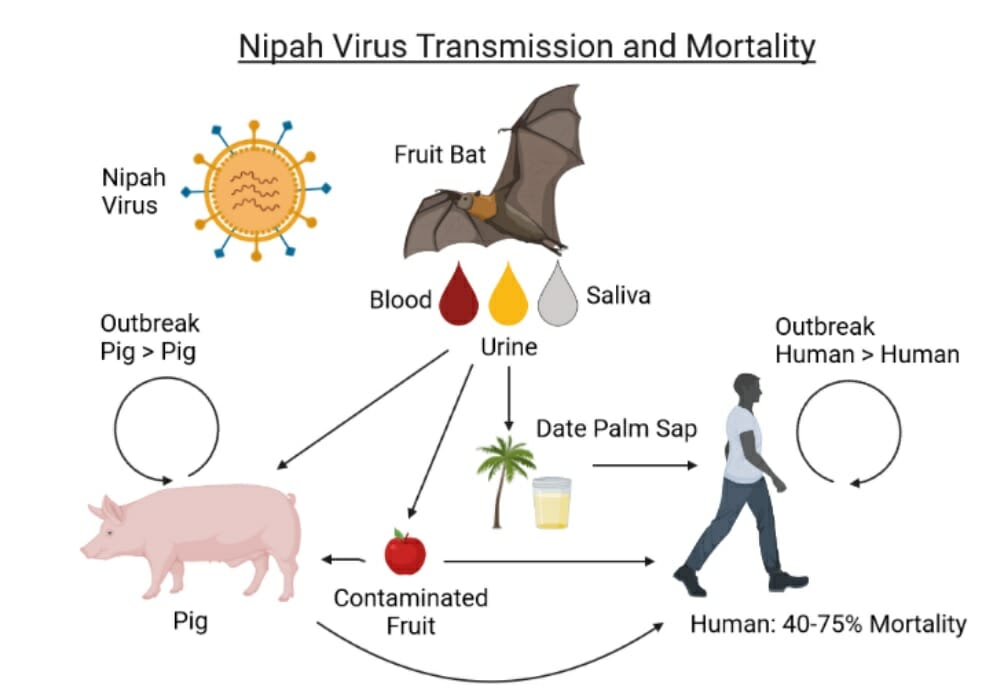
The Nipah virus: A bat-borne virus posing a potentially “great threat” to both humans and livestock, that was lacking a vaccine
Not among the list above -yet- is the Nipah Virus, a priority pathogen designated by the WHO and categorized by the U.S. Centers for Disease Control (CDC) as a Category C Bioterrorism agent. The Nipah Virus is a bat-borne virus that spreads to both humans and livestock, causing febrile encephalitis.
It was first discovered in 1999 following an outbreak of the disease in pigs and people in Malaysia and Singapore, resulting in more than 100 deaths, with 1 million pigs culled to control the outbreak, and enormous impact on farmers and communities.
There have been several subsequent outbreaks between 2001 and 2005 in Bangladesh and as recently as August 2021 in Kerala, India, indicating its extensive and expanding reach in South Asia and Southeast Asia.
For most pharmaceutical companies research costs, odds of success, and potential return on investment, are factors that make a virus an unlikely vaccine candidate. Yet one biotechnology company, Public Health Vaccines (PHV), took on the Nipah challenge in partnership with Crozet BioPharma as together they had already “helped to advance a vaccine against Ebola which is now approved for use,” as Dr. Thomas Monath said (he’s with Crozet BioPharma and Senior Advisor to PHV).
This team has made significant progress with Nipah, specifically in just announcing the start of a Phase 1 clinical trial to evaluate the safety and immunogenicity of the company’s single-dose Nipah vaccine. They reached out to create a public/private partnership with the international donor organization, “Coalition for Epidemic Preparedness and Innovations” (CEPI), which has provided substantial funding such that it could facilitate development through Phase 2 clinical trials, including supportive non-clinical and manufacturing activities.
A One Health Prevention Opportunity
The Nipah Virus represents potentially a major threat, an infectious disease of animal origins, deadly to humans, and capable of spreading to new environments, having already been found in pockets of one of the most densely populated regions in the world. Getting a Nipah vaccine developed and then produced combines both “prevention” and “preparedness” – a win-win situation for us all.
Having a Nipah Virus vaccine in place before major infections break out on a massive scale is the essence of “prevention” and an integral part of an effective One Health approach. We need it. We should not ever have a repeat of Covid or Ebola.
Editor’s Note: The opinions expressed here by Impakter.com columnists are their own, not those of Impakter.com. — Featured Photo: Close up of a scientist using a microscope, December 11, 2021 Source: cc by 2.0 Nenad Stojkovic









