Half the world population cannot access health services but progress has been made in Low and Middle Income Countries: Kudos to them.
In 2017 the United Nations General Assembly (UNGA) adopted resolution A/72/l.27 establishing December 12th as Universal Health Coverage Day (UHC Day), to be celebrated annually – a good time to review and assess results towards achieving the health goals of Agenda 2030, in particular Sustainable Development Goal 3 “ensure healthy lives and promote well-being for all ages”. Overall, the assessment is not encouraging, global health is in bad shape. But there are some signs of progress, in particular in the public health sectors of low and middle income countries. Not so good in developed countries. Let’s take a closer look.
The data to assess where we globally stand is available thanks to the efforts of UN statistical services. The data allows the UNGA to consider and continue to regularly review with a strong degree of confidence the state of non-communicable diseases, antimicrobial resistance, pandemic preparedness and the progress made towards the health goals of the Sustainable Goals (SDGs).
The UN Sustainable Development Goals Knowledge Platform puts SDG 3 progress this way, starting with the good news:
“Major progress has been made in improving the health of millions of people, increasing life expectancy, reducing maternal and child mortality and fighting against leading communicable diseases.”
And now the bad news.
Half the global population does not have access to essential health services
As the UN Secretary General’s report puts it in a special edition:
“…progress has stalled or is not happening fast enough with regard to addressing major diseases, such as malaria and tuberculosis, while at least half the global population does not have access to essential health services and many of those who do suffer undue financial hardship, potentially pushing them into extreme poverty.”
Tuberculosis (TB) happens everywhere, and 1.5 million people died from TB in 2018. But the largest number of new TB cases occurred in the South-East Asian region (44% of new cases), followed by Africa (24% of new cases).
The problem of access to essential health services affects all countries, even the more developed ones, including the United States where, according to some sources (PBS), up to 44 million Americans are uninsured and another 38 million have inadequate health insurance, thus putting them at risk.
In the video: Germany’s health-care system spends nearly half as much as the United States but still manages to cover 100% of its population through a mix of public and private insurance schemes. Source: CNBC, 24 November 2019
The UN report continues, noting that:
“Concerted efforts are required to achieve universal health coverage and sustainable financing for health, to address the growing burden of non-communicable diseases, including mental health, and to tackle antimicrobial resistance and determinants of health such as air pollution and inadequate water and sanitation.”
Such “concerted efforts” are key to achieving SDG 3 which is specific to health, but there’s more to it. We know that virtually all other sixteen SDGs bear on how successful or unsuccessful a country or region is in having desired health outcomes. Thus this crisp SDG statement is important and balanced to be sure, implicitly encompassing pandemic preparedness, zoonotic diseases, the One Health approach that recognizes that the health of people is connected to the health of animals and the environment – hence climate action, reduced inequality, peace justice and strong institutions. And the many aspirational efforts all countries are to work toward. The graph below provides a picture of the interrelationships:
Multiple efforts have been and are being undertaken to collect data and build country specific evidence bases to better understand the performance and unmet challenges by countries.
Most recently in October 2019 the “Global Health Security Index: Building Collective Action and Accountability” was released. It is the first massive and comprehensive assessment and benchmarking of health security and related capabilities across 195 countries that make up the countries under the World Health Organization’s International Health Regulations. This document, along with many others, reflects what national health sectors are doing, sometimes well, sometimes not-so-well. Here is the 2019 map of the state of world preparedness for epidemics and pandemics:
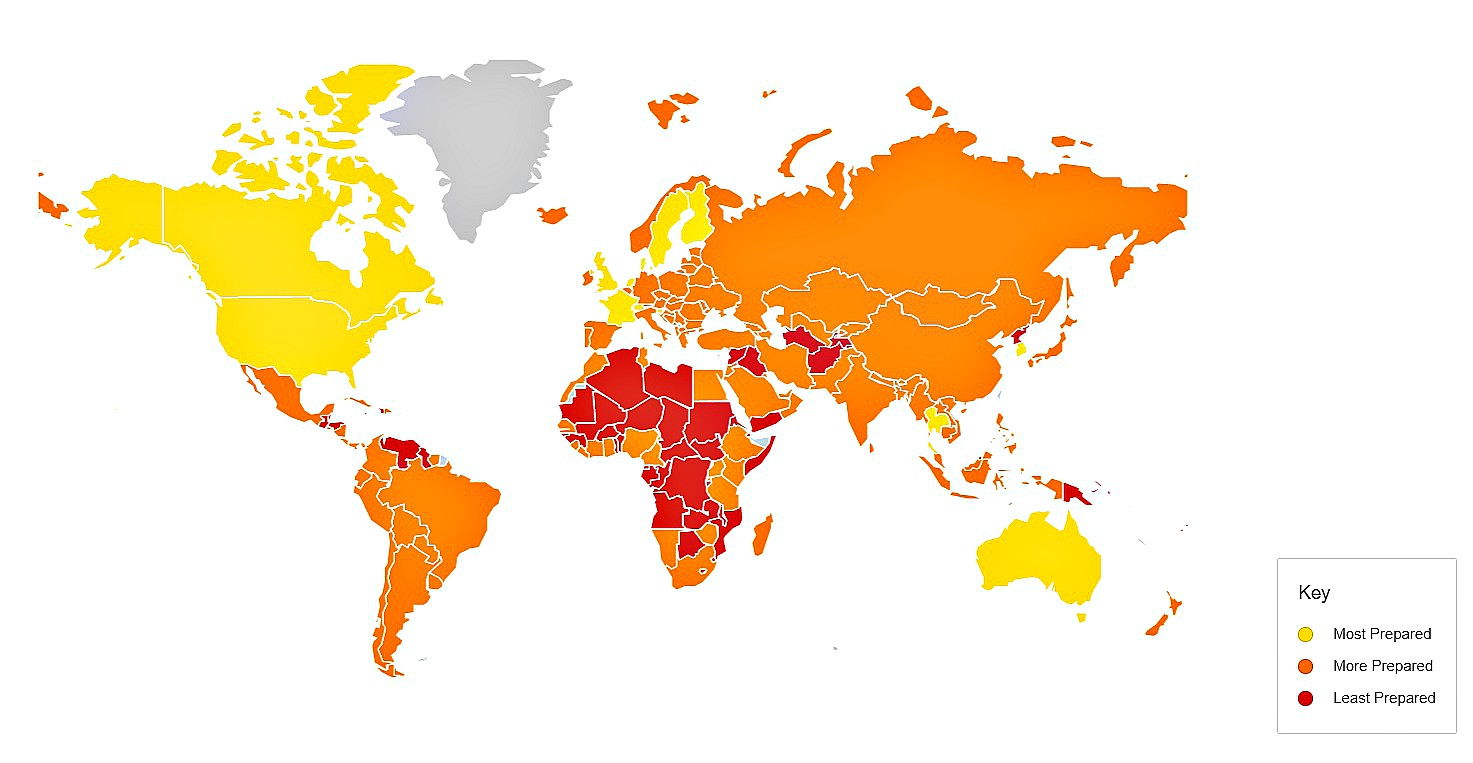
Recognizing Those Responsible for Health in Low and Middle Income Countries
As we look to December 12, 2019 UHC Day celebrations, we need to recognize on whose shoulders the main burden for health outcomes rest. This is an opportunity to consider and sympathize with what low and middle income country senior most career health officials face as they conscientiously seek to navigate global desires and address local realities. As the above GHS Index map indicates, the countries facing the most serious challenges are in Africa. with some hot spots across the world, mostly in the Middle East.
Typically a health secretary general or minister has so many competing interests and pressures that make three dimensional tic-tac-toe look like child’s play. Major internal influencers include people of wealth or political influence who are often more interested in hospital care than basic services for all. Constituencies in urban and semi-urban environments usually have greater access to the decision makers than rural communities, unless and until these communities organize and become vocal and visible.
Health staffing is another headache, with too few professionals trained, recruited, deployed and kept within the public sector in the country. And then there is the intense intersectoral competition for limited public sector resources with national security, education, infrastructure, to name a few.
Finally, we come to the donor community, whether multilateral, bilateral, non-governmental, either for or not-for-profit, with separate programs, projects, reporting requirements and hand-holding. In short, these often underappreciated officials face a plethora of competing interests, policies, and programs.
There are times when those of us on the outside, need to make the effort to commend those on the inside. December 12, 2019 UHC Day is just such an occasion.
EDITOR’S NOTE: The opinions expressed here by Impakter.com columnists are their own, not those of Impakter.com – Cover photo: Community health worker gives a vaccination in Odisha state, India. Community health worker, Rebati, gives babies like Adilya, polio and other life saving vaccinations for at least the first year of their lives. Source: DFID, UK Photo: Pippa Ranger/DFID










