They call it a “code R” in some pediatric emergency departments. It is a way to protect the privacy of our child and teen patients. It is also a way to clinically detach, distance us from the horror of what lies in the exam room. Code R: Rape or sexual assault. There is a protocol for that, a checklist. On the other hand, the words – rape, sexual assault – precipitate emotional reactions; they stop us in our tracks, and force us to come to terms with the reality that terrible things can and do happen to the most vulnerable members of our society.
Although national estimates vary widely, as many as one in four girls and one in six boys experience some form of sexual abuse in childhood. Older teenage girls, from 14 to 18 years of age, are at particularly high risk of sexual violence: nearly 12% report that they have been forced to engage in sexual intercourse. As devastating as these statistics are, they likely underestimate the true incidence of sexual assault on children.
While as many as nine in ten child victims of sexual assault never have recourse to the criminal justice system or seek medical care for the assault, emergency departments are often the first place of refuge for the minority of sexually assaulted children who do seek care. Even for those children who do not explicitly admit to the assault, physicians are important screeners for and mandatory reporters of any suspected cases of abuse. Physicians and nurses are trusted to be nonjudgmental, supportive and competent.
Unfortunately, even when the stakes are as high as they are in pediatric sexual assault, physicians frequently err; they fail to recognize and fail to appropriately treat these children.
I was recently at a conference in a room full of emergency medicine physicians. The speaker had us all stand, and then she asked us to sit down if we ever might have missed a case of sexual assault. Some looked down at their feet as they took a seat. Others scanned the room, making sure that they were not alone in their admission of missed diagnosis. After a few moments, not a single person in the room remained standing. We all shared the collective shame of knowing that we could have done better and that we should do better, next time.
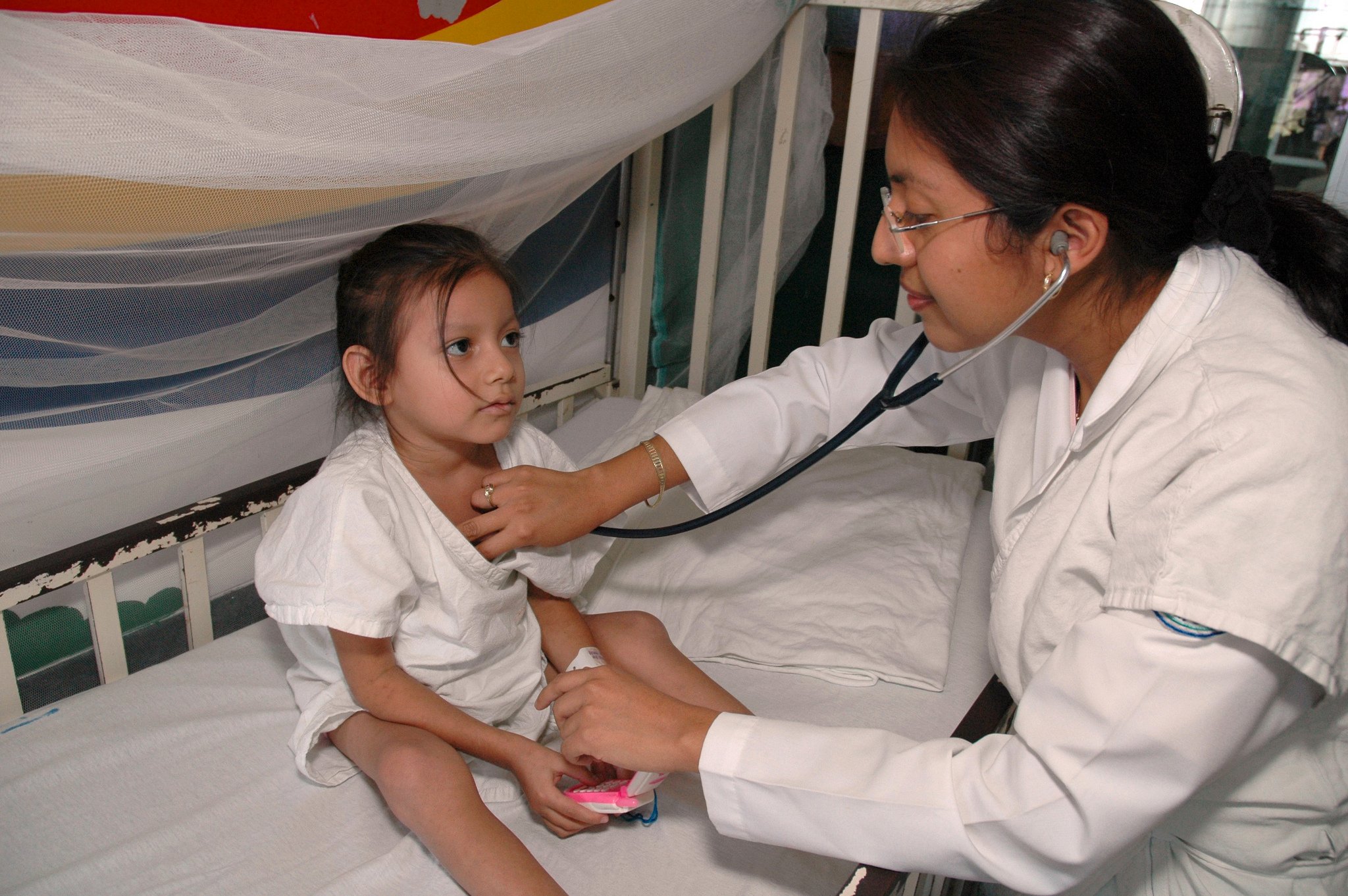
In the Photo: A physician examines a young patient. Photo Credit: Flickr/PAHO-WHO
A recent study asked emergency medicine providers about their barriers to recognizing and reporting child abuse. “I’m a trusting person,” one provider reported, “I want to believe what people tell me.” Another provider admitted that a parent that looks “put together” would seem less suspicious and might not prompt any deeper questioning into potential abuse. Providers also admitted that the cumbersome process of reporting abuse discourages them from doing so, especially in a busy emergency department.
The whirlwind of workflow in emergency departments predisposes medical providers to the error of missing cases of pediatric sexual abuse. The objective evidence of a head CT scan can confirm stroke, laboratory tests can suggest heart attack. And when these life-threatening conditions are scattered throughout the department, staring you in the face, it can be easier to assume that the subtler but equally devastating diagnoses – abuse, assault, addiction – are not there.
The sheer volume of patients and the need to provide time-sensitive medical care also predispose emergency physicians to judging patients and parents based on appearances. Pattern recognition is an essential component of practicing emergency medicine. When I see a woman with difficulty breathing who recently took a long car ride, my brain jumps directly to ruling out a blood clot in her lung. When I see an older man with sharp chest pain that travels to his back, I worry about a possible tear in the major blood vessel that comes out of his heart. And when I see that a child is brought to the hospital by a father dressed in a nice suit, perhaps I am slower to think abuse than when the man is disheveled and disorganized. But, pediatric sexual assault is not limited to a certain demographic. Persons of all gender, age, race, and socioeconomic status perpetrate these crimes.
Related Articles: “WOMEN MAKING THEIR OWN FERTILITY DECISIONS” by SHEENA DASANI
“THE TRUTH ABOUT BURNOUT AND SUICIDE AMONG PHYSICIANS” by ALESSIA MINICOZZI
When asked about barriers to recognizing child abuse, another emergency medicine provider worried, “If nothing comes of [the report to Child Protective Services]…you’re scared…thinking, I just bothered that family for no reason based on my assumptions.” I have never seen an emergency physician, on the other hand, agonize over inconveniencing a patient if medical testing came back negative for a disease such as appendicitis or pneumonia.
Even when the sexual assault is recognized, the majority of physicians fail to treat the children appropriately. The U.S. Centers for Disease Control and Prevention recommend that sexual assault victims be given medications to treat them for sexually transmitted infection and to help prevent pregnancy. Failing to provide these treatments puts patients at risk for an uncomfortable and potentially incurable infection. It puts girls at risk for infertility, at one end of the spectrum, or a traumatic and unintended pregnancy, at the other. Victims of sexual assault don’t always follow up, so their initial presentation to the emergency department might be their only chance to be treated.
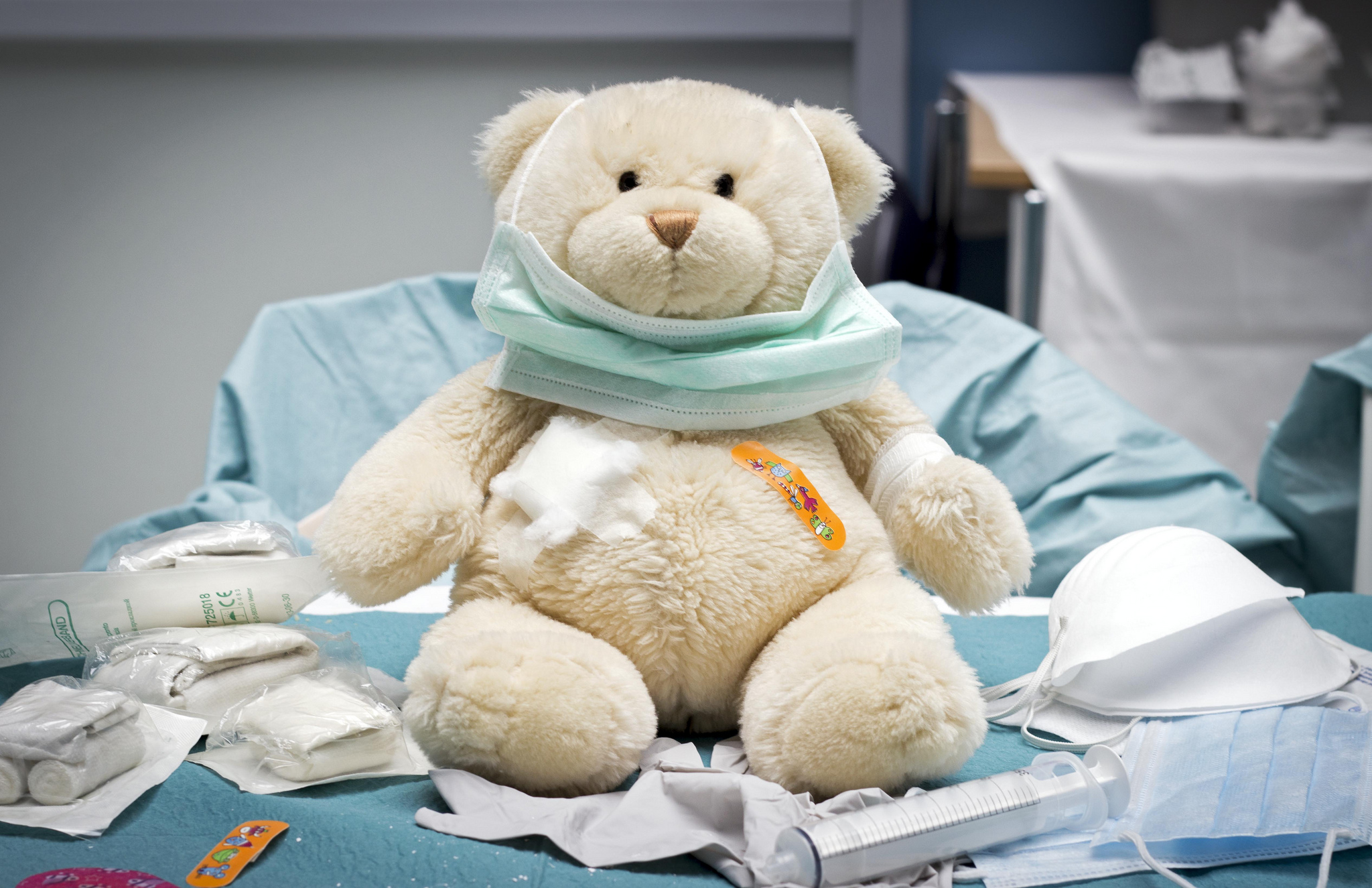
In the Photo: The Teddy Bear Hospital introduces children to appointments. Photo Credit: Flickr/Christiaan Triebert
Barely one third of sexually assaulted teens, however, receive the recommended medications in pediatric emergency departments. At some hospitals, rates were as low as zero percent.
When it comes to our most vulnerable patients, these children who have been sexually victimized by their caregivers or peers, we can do better. But, in an environment punctuated by alarm bells for critically ill patients, where physicians and nurses are stretched to full capacity, how can we improve?
One solution to this problem is the use of clinical decision pathways. Emergency department pathways are becoming increasingly popular: hospitals draw on local expertise and national guidelines to create simple “yes/no” decision trees that help the provider efficiently determine the most likely diagnosis and most appropriate course of action. For example, for a child presenting with a simple asthma flare, the algorithm might ask about the severity of previous asthma attacks, the child’s blood oxygen level, and the breathing rate in order to guide the physician towards the best medications to try first.
As many as one in four girls and one in six boys experience some form of sexual abuse in childhood.
For pediatric sexual assault, the pathways are inherently more subjective, requiring the physician to comment on his or her degree of suspicion for sexual assault. Despite their imperfections, the pathways can help providers approach pediatric sexual assault in a standardized way. Especially for young providers or trainees, these pathways can help to validate their concern and make the accusation of assault seem less personal. However, one recent survey found that only one in three pediatric hospitals was currently using a pathway to assess for and manage sexual assault.
The use of specialized teams, sometimes called CPTs (Child Protection Teams) or SCAN (Suspected Child Abuse and Neglect) teams, is another way that emergency departments have approached the problem of detecting and managing pediatric sexual abuse. These teams, composed of members such as physicians, nurses, and social workers, can function without competing distractions: their sole responsibility is to those children who have been flagged as at-risk for some form of abuse. Emergency physicians can trade a prolonged and potentially painful conversation with the family for a quick page to the SCAN team. These teams are also underutilized, however. Less than two thirds of pediatric emergency departments have access to this resource.
In the Photo: A banner noting Child Abuse Prevention Month. Photo Credit: Flickr/Daniel X. O’Neil
In addition to aiding in diagnosis, specialized teams and decision pathways improve rates of appropriate treatment. However, even in the pediatric emergency departments with the most resources, barely over half of the children were given the necessary medications to prevent pregnancy and infection.
Pathways and teams, then, aren’t enough. We need a paradigm shift in how emergency physicians approach the horrific diagnosis of pediatric sexual assault.
In medical school, I was exposed to dozens of hours of lectures on cancer and heart disease – important, leading causes of death. I can only recall a couple of lectures that even touched on violence and abuse, on the other hand, with even less time devoted to understanding how these issues affect and victimize children.
In sexual abuse, however, the paradigm seems to be flipped. Physicians worry about inconveniencing or embarrassing families if the formal evaluation comes back negative for child abuse or sexual assault.
In the hospital, too, my education on recognizing and treating pediatric sexual abuse has been limited. Supervising physicians have steered me away from the “Code R” patients. They want to help prepare me to evaluate common and challenging medical conditions such as asthma or infection, but how then will I build the base of experience to approach sexual abuse or assault? I have also had well-intentioned supervising physicians who ask me to wait outside the room while they talk to my patient and his or her family about the concern for abuse. The physicians do so to try and make the discussion as private and comfortable as possible, but where will I learn how to navigate these delicate and devastating conversations? Efforts to do better by our patients must start early in physicians’ training.
Beyond improved education and increased awareness, we must shift from seeing sexual abuse as a condition that must be “ruled in” to a condition that must be “ruled out.” The paradigm in emergency medicine is generally to exclude life-threatening conditions before a patient can be safely sent home. There is a saying that trainees are taught: “If you think about ordering a test, just do it.” In other words, if you are concerned enough about a diagnosis to have even the fleeting thought of it, you should probably go ahead and test the patient. If the test is negative, at least you have given yourself and your patient the peace of mind of knowing that you didn’t miss something.
In sexual abuse, however, the paradigm seems to be flipped. Physicians worry about inconveniencing or embarrassing families if the formal evaluation comes back negative for child abuse or sexual assault. They worry about disrupting the physician-patient relationship or alienating families.
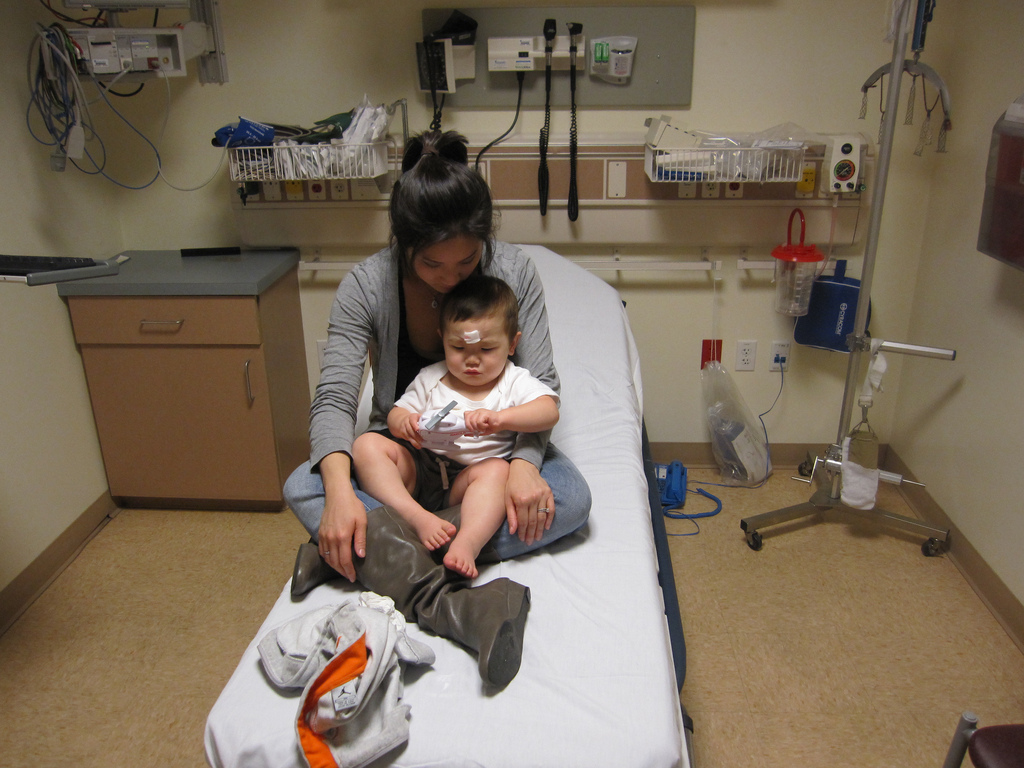
In the Photo: A child waits in the ER to be treated. Photo Credit: Flickr/jencu
In recognition of physicians’ reluctance to have certain difficult conversations, some emergency departments are moving towards screening every single patient for suicide and addiction. There is an acknowledgement that patients might not necessarily “look like” they’re alcoholics or depressed, but every patient is at risk for these conditions. Patients simply click through a few questions on the computer while they wait for the physician to come in, and the results are automatically added into their medical chart and flagged if worrisome. A similar approach could be taken for pediatric sexual assault, but research is needed to develop and test a screening tool for this purpose.
Even once the assault is recognized, another paradigm shift is needed to ensure appropriate treatment. In emergency medicine, we are taught to bucket patients as “sick” or “not sick.” Is the patient A) potentially critically ill or B) medically stable and able to be sent home? A child victim of sexual assault does not fall squarely into either category. Once the physician ensures that the child is safe at home, there seems to be a reluctance to provide further treatment. There is, perhaps, an assumption that the child can later be treated by his or her regular pediatrician. But these are among the most vulnerable members of society, potentially victimized by a trusted caregiver or peer. We owe it to them to do everything we can to protect them – from repeat violations, from life- or fertility-threatening infection, and from a devastating future pregnancy. This is too important of a role to be passed on to another physician in the hopes that the child will seek medical care later.
To err is human, but to fail our young patients in this way is unacceptable. Systems of care can be improved, but to truly do better when our children need us most, we must change the way physicians learn and think about pediatric sexual assault.