Today, there are many hotly-debated issues that polarize politics in America and the world alike. Healthcare should not be one of those issues. It is not difficult to see that the current American healthcare system is critically flawed when one’s financial situation is greatly influenced by the state of their health. In one survey (Washington State), cancer patients were found to be 2.65 times more likely to go bankrupt than people without cancer.
It is only indicative of the dire state of American healthcare that people resist the very first stage of emergency medical treatment: the ambulance ride. A short ambulance ride can leave a person straddled with thousands of dollars in medical bills. With the advent of ride-sharing services such as Uber and Lyft over the last few years, people have found new ways to circumvent the ambulance ride.
In fact, in 2017, a paper written by two economists from the University of Kansas, revealed that following the deployment of UberX services in a U.S. city, the number of ambulance trips in those cities decreased by an average of 7%. This was due to the fact that low-risk patients started opting for cheaper emergency transportation, resulting in the reduction in net ambulance rides in the cities.
Call9, a Brooklyn-based startup founded in 2015, came up with a way to cut out the costly ambulance ride—and more importantly the entire trip to the hospital—all together. However, instead of focusing on the average person, they catered their services to the patient population that needed them most: people in nursing homes.
Research conducted in 20 nursing homes in 2010 concluded that 68% of the hospitalizations observed during the period of research could have been avoided. Moreover the research confirmed that for older patients, trips to the hospital were in many ways detrimental to their health, due to the delirium and discomfort that they had experienced during the ordeal. A nursing home can also be legally responsible for personal injury or medical malpractice when an act of negligence, neglect, or abuse on the premises ends up causing harm to a patient or resident. If this is happening to your loved one, you can contact a nursing home abuse lawyer in new york for legal help.
In the photo: A Call9 technician provides a demonstration of the company’s technology, with Co-Founder and CEO Timothy Peck watching on. Photo Credit: Call9
Upon further research, it was identified that about 19% of all ambulance transfers to the emergency department come from nursing homes. Nursing homes were the largest single source of 911 calls and transfers to the emergency department.
Led by Dr. Timothy Peck, Call9 has sought to reinvent the 911 call by utilizing telemedicine and producing portable technology that provides the functionality of an ambulance, in order to allow for bedside treatment and avoid unnecessary hospitalization. As a result of their efforts, the startup secured funding from the renowned YCombinator, along with many other venture capital firms. They since have successfully completed their Series B.
Garrett Gleeson, the Chief of Staff & SVP of Government and Public Relations at Call9, sat down with Impakter Magazine to discuss the journey of the start-up, its medical and economic impact, and its plans going forward.
What was the inspiration for the founding of Call9 Solutions?
Garrett Gleeson: An everyday challenge that Tim Peck saw during his time working in the emergency department was nursing home patients who were not receiving great care there. They would arrive without their advocate and without any medical history, and as a result they had to be tested for everything under the sun as doctors would to figure out what it was that had brought them there. They would then get admitted to the hospital and spend three to four days in the hospital before going back to the nursing home. That cycle would repeat itself another five to six times a year, sometimes more.
Besides old age, why are so many patients who come to the emergency room from a nursing home?
G.G.: To get to the root of the problem, he went to live in a nursing home for three months in order to really understand why this was happening—why so many patients were being sent to the emergency department from nursing homes. As a result of his observations, he identified three primary drivers for the issue.
One: nursing home nurses are well-trained at providing chronic care but often times aren’t necessarily trained for acute care. Additionally, their bandwidth is limited; the average nurse-to-patient ratio in nursing homes is 1:36. When any patient has an acute change of condition, the nurse has another 35 patients to attend to as well. The default response is to call 911 and transfer the patient to the emergency department.
Two: diagnostics in nursing homes are sparse. They are for chronic care, not acute care. Means of diagnosis such as EKGs and lab tests take 24 hours to 48 hours to return which doesn’t work for acute changes of condition.
Three: doctors are not always available in nursing homes during nights, weekends, and holidays. There also isn’t a constant need for a doctor to be present as long-term patients only need to be seen once a month in nursing homes. The high-level decisions that doctors can make are only required in emergency situations.

In the photo: A demonstration of Call9’s service in action. Image Credit: Call9
How does your service work?
G.G.: We place a first responder—generally an EMT or a paramedic (anyone with emergency training experience)—onsite. If an emergency occurs, they go to the patient’s bedside with a suite of diagnostics that is always at the location. This allows to conduct an array of tests that provide results in two minutes or less.
The first responder also has our app and immediately connects the patient to our remote emergency medicine physician. This doctor is at home on their laptop. They can see our patient and they can see our first responder. Thanks to the suite of diagnostics they can see all the patient’s real-time vitals on their screen and we also have integrations which allow them to see the facility’s electronic medical record. Access to medical records is a luxury that you rarely have if you are a doctor working in the emergency department.
In this way we are able to diagnose and deliver care to the patient with the hand of the first responder and the mind of the doctor, allowing patients to remain in the nursing home and avoiding the hospital.
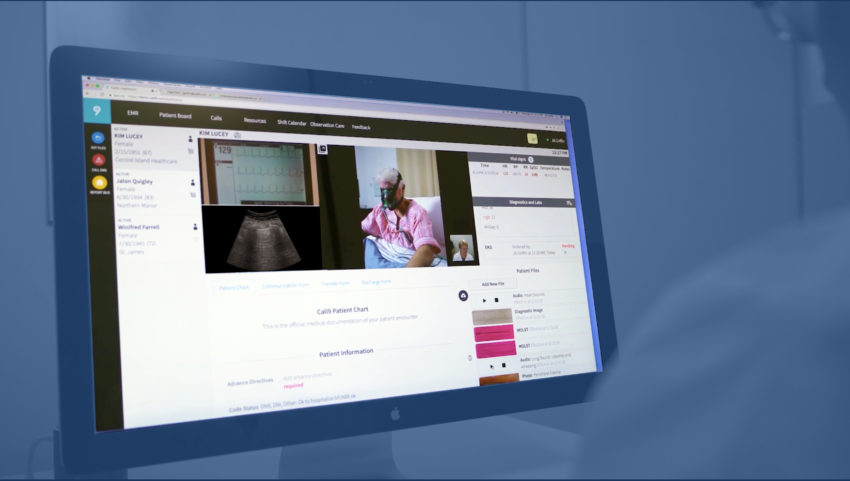
In the photo: A brief glimpse at the interface seen by the doctor when assessing their patient. Photo Credit: Call9
Can you share any figures regarding the effectiveness of your service in accomplishing your mission of reducing unnecessary hospitalizations?
G.G.: In the fall of 2016, we had a third-party economics firm track our work for a number of months and they identified that we saved insurance payers 8 million dollars a year in every 200-bed nursing home that we are in. Further, it was found that Call9 has decreased unplanned hospital visits and ambulance utilization by over 50% in skilled nursing facilities.
RELATED ARTICLES:
 Smart Vision Labs: Harnessing Telemedicine to Provide Affordable and Accessible Eye Care for All
Smart Vision Labs: Harnessing Telemedicine to Provide Affordable and Accessible Eye Care for All
 Good Zing? The Future of Universal Healthcare?
Good Zing? The Future of Universal Healthcare?
 The 203 Companies Taking Impact Improvement to Heart
The 203 Companies Taking Impact Improvement to Heart
 Sustainable Energy Can Power A Health Revolution
Sustainable Energy Can Power A Health Revolution
What are some of the benefits for doctors working via telemedicine?
G.G.: This is a unique way of practicing medicine so there is a lot of interest in this type of work from the physician community. When you are working in the emergency department you are on your feet for the entirety of a shift, it is hectic, and it is mainly a young person’s game. Therefore, it is appealing for older physicians, stay-at-home moms, and physicians with physical limitations for one reason or another.
Do you see a general trend towards telemedicine becoming more commonplace in medical practice and what changes must occur for that to be possible?
G.G.: That is the biggest limitation to the growth of Call9 solutions, and at Call9, we are not the only ones in the country doing this, and there would be a lot more people doing this if Medicare were to reimburse for this solution. I have met with over 200 congressional offices over the past year and we have been spending a lot of time on Capitol Hill. From 2000 to 2018, there were zero telemedicine bills that were passed into law. In 2018 there were five. The trend towards telemedicine is a big transformation that is occurring in healthcare.
…congressional leaders get it—to be clear. This is a 40 billion dollar problem that we are talking about…
Legislation has been crafted to reimburse physician groups that use telemedicine to treat patients in nursing homes to avoid hospitalization. And congressional leaders get it—to be clear. This is a 40 billion dollar problem that we are talking about, when it comes to unnecessary transfers to the emergency department. This would allow groups that use telemedicine to grow around the country and get adopted in nursing homes around the country. This is a chance to create transformation in the way that we care for our oldest and sickest patients in the country.
Are there any other applications for your service outside of a nursing home?
G.G.: The service can definitely be used at sporting events or in prisons or in resorts. There are many ways in which the technology can be used, but our focus is on the highest utilizers of the emergency department which come from nursing homes. There are 15,600 nursing homes in the United States and there is just a huge opportunity to deploy this technology for this patient population. Avoiding hospitalization for this patient population is the most impactful way to use the technology and that is our focus for the foreseeable future.

In the photo: Some facts about nursing homes in the U.S. Image Credit: Call9
Who are some of your partners and where do you plan to expand to in the future?
G.G.: Using the information that we gathered about our services, we were able to quickly get into contracts with the biggest insurance payers in New York, including United Healthcare and Empire BlueCross BlueShield. Since then we have partnered with many other big national and local payers. From there we wanted to get into more nursing homes, raise our Series B, and start expanding through lower New York. Now we are also in Syracuse and we are planning to move into Albany in March.
Cover Photo Credit: Call9
_______________________________________________________________________
EDITOR’S NOTE: The opinions expressed here by Impakter.com columnists are their own, not those of Impakter.com.









