EDITOR’S NOTE: THIS PIECE IS AUTHORED BY COURTNEY STORM. AN AUTHOR OF PEER-VIEWED PUBLICATIONS ON TOPICS RANGING FROM FINANCIAL CONFLICTS OF INTEREST TO THE MEDICAL AND LEGAL IMPLICATIONS OF CANCER GENETIC AND GENOMIC TESTING. COURTNEY HAS WORKED FOR RESEARCH SOCIETIES, NATIONAL INSTITUTES AND SERVED ON VARIOUS BOARDS.
We’ve all been there, or at least seen the TV commercials: a sudden, midnight bout with the flu leads, inevitably, to a late-night trip to CVS for Advil Cold and Sinus. Allergies flaring up? Pass the Claritin! Kids have strep throat? Thank goodness for amoxicillin. We depend on over-the-counter and prescription drugs to treat every day ailments, and take for granted that there will be more potent drug regimens available to us if we are diagnosed with something more serious (e.g, cancer, heart disease, diabetes).
Yet we do not give much thought to how these drugs evolve from ideas tested in a lab to the helpful medications we take. The key questions are:
How are drugs researched and tested? What does it mean for a drug to be FDA approved?
In short, is FDA approval an important safeguard to preserve, or a regulatory obstacle that should be minimized to expedite the drug approval process?
1. DRUG DEVELOPMENT
The drug testing and drug development process includes laboratory research, animal testing, and human clinical trials. Laboratory research may target a specific medical need, investigate new uses for existing drugs, or explore how new compounds work against a broad swath of diseases. The latter is called “basic” or “bench” research, and it is often a bust; very few research compounds show enough promise to warrant further investigation.
IN THIS PHOTO: “Generic Drug Testing Research” – PHOTO CREDIT: Flickr/FDA photo/Michael J. Ermarth
For this reason, drug companies are reluctant to support basic research, and the amount of public funding is often subject to debate.
However, basic research lays essential groundwork for medical advances that targeted research does not. For example, a basic study of neurotransmitters led to the discovery of serotonin receptors and the eventual development of Selective Serotonin Reuptake Inhibitors (SSRIs), i.e. Prozac. The anti-tumor effects of tamoxifen were discovered only after it failed company sponsored research targeting contraceptives and fertility drugs, and AZT was initially tested as an anti-cancer drug. After basic research, animal testing is used to show how drugs work and to identify negative side effects.
PHOTO CREDIT: PIXABAY
These results are submitted to FDA as part of an Investigational New Drug (IND) application. If FDA determines the drug is safe to be tested on people, researchers can proceed with human clinical trials:
- Phase I clinical trials: are designed to show that a drug is generally safe and how it works.
- Phase II trials: look at whether the drug is active against a certain disease, at what dosage, and;
- Phase III trials: compare the drug with standard treatment to see if the new drug is more effective against the disease, or has fewer negative side effects.
Clinical trials must follow detailed written plans that describe research goals, methods, procedures, risks, benefits, and criteria for determining which patients can safely participate. Clinical trials are subject to laws and ethical standards that protect participants. Federal regulations, known collectively as the Common Rule codify a long history of human subject research protections dating back to the Nuremberg Code. These rules require that:
- Clinical trials pose minimal risk to participants.
- Ensure that risks are reasonable with respect to possible benefits, and;
- To require additional steps to protect especially vulnerable populations (e.g; children, pregnant women, prisoners).
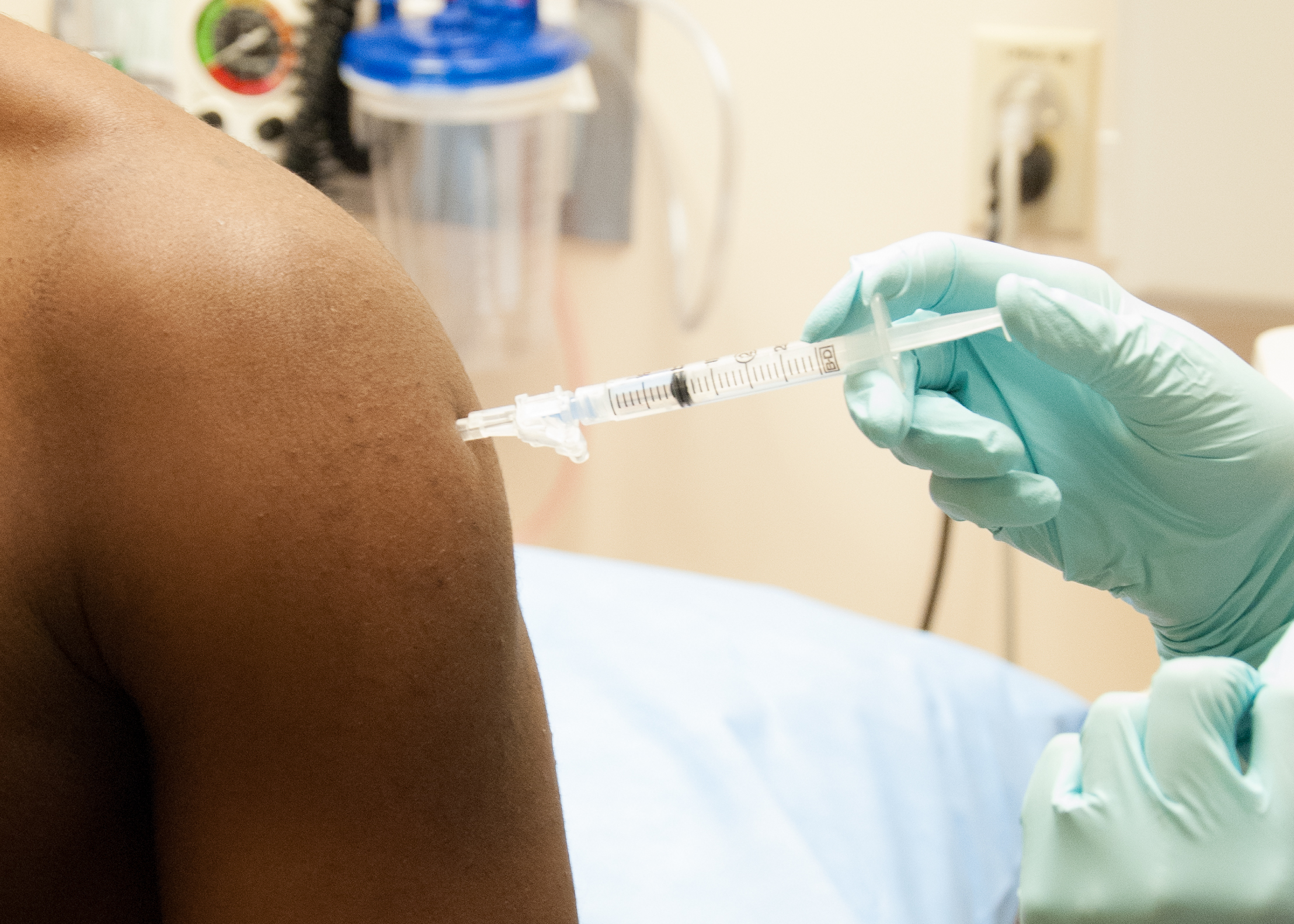
Participants must understand the study, the potential risks, and that—unlike medical treatment—research is not designed to benefit them directly. Institutional Review Boards (IRBs); groups of scientists, doctors, nurses, lawyers, ethicists, clergy and community members—approve and monitor clinical trials to ensure these standards are met.
IN THIS PHOTO: “Study Participant Receiving Investigational NIAID/GSK Candidate Ebola Vaccine” PHOTO CREDIT: Flickr/NIAID
2. FDA APPROVAL
Once clinical trials are complete, data is submitted to the Food and Drug Administration (FDA) for review. Drugs are approved if they are both safe and effective against a specific disease. Only FDA approved drugs can be sold and marketed in the U.S.
Though the FDA approval process is often criticized as slow-moving, the median time from data submission to approval was just over 10 months. This is considerably faster than approval in Canada or Europe.
In addition, FDA offers “fast track” approval pathways for drugs that treat serious or life threatening conditions, substantially improve upon existing treatments, or fill un-met medical needs. Fast tracks allow researchers to consult with FDA earlier and more frequently; evaluate data on a “rolling” basis; and base approval on data showing a drug is likely to be beneficial, rather than waiting longer for direct evidence. For example, a breakthrough oncology drug can be approved based on data showing progression free survival, which is a strong indicator of an overall survival benefit.
3. EXPEDITING ACCESS TO NEW DRUGS
Even with FDA fast tracks, the drug development process—from initial clinical testing to FDA approval—can take a decade
This is, of course, too long in the eyes of stakeholders like drug companies, eager for a return on investment in drug development, and patients who want faster access to new drugs.
These groups may support policies that mitigate or circumvent drug approval requirements. One example, the 21st Century Cures Act (2016), requires FDA to explore the use of “real world evidence” (RWE) gathered outside of clinical trials to support new drug approval. Potential sources of RWE include; electronic medical records, insurance claims, and patient registries.
Advocates believe collecting RWE is more efficient than conducting lengthy clinical trials, and more accurately reflects the realities of clinical practice. However, sources of RWE vary in quality and format, making data difficult to analyze. In a recent New England Journal commentary, FDA leaders stand by the scientific rigor of clinical trials necessary so that a drug is both safe and effective, noting that RWE is promising but unlikely to yield “quick wins.”
IN THIS PHOTO: “Signing of medical cannabis ordinance in Seattle by Mayor McGinn” PHOTO CREDIT: Flickr/Jen Nance/Office of the Mayor
A second example, “Right-to-Try” laws, allow terminally ill patients to access investigational drugs after Phase I testing, well before FDA approval.
Thirty-one states have already passed right-to-try laws, and a proposed federal law will likely gain traction in the Trump administration. The Vice President and several people on the short list for FDA Commissioner support right to try laws and, in his address to Congress on February 28th 2017, the President advocated for “slashing restraints” at FDA and beyond that keep [medical] advances from reaching those in need.
Related article: “PRESIDENTIAL BIOETHICS: VALUING PRODUCT AND PROCESS”
However, medical, legal and ethical experts criticize right-to-try laws as ‘feel good’ legislation that can harm seriously ill patients.
First: Right-to-try laws do not (possibly, legally, cannot) require companies to provide the drug. Rather, they encourage companies to comply voluntarily by providing immunity from law suits arising from injurious side effects and precluding adverse events from counting against a drug’s application for approval.
Second: Patients who receive the drug may experience significant side effects and no benefit. Even after a Phase I trial, researchers do not know if a drug works, what dose to give, or the potential side effects (which could be more severe in very sick people).
Right-to-try laws also seem gratuitous considering FDA’s expanded access program, through which terminally ill patients can receive investigational drugs outside of clinical trials.
Right-to-try advocates say; “FDA’s consideration of expanded access requests are too slow”, and “requests are rarely granted.”
However, FDA recently streamlined its expanded access application process and reports that requests are considered quickly (within four days), and are almost always (99 percent) granted.
4. MOVING FORWARD
It has been said, more than once (including by Toby Ziegler in an episode of the West Wing), that it is the everyday processes we rely on without much thought that cause the most upheaval when they stop working. Expediting access to new drugs is an important goal, and it is incumbent on FDA to make sure its regulations are streamlined and efficient.
However, there is a difference between streamlining and gutting, or circumventing, requirements that protect public health and safety. This line should be respected, and FDA allowed to do its job.
Moving forward, streamlining efforts must include other barriers to drug access, including the high cost of prescription drugs and insurance coverage determinations. A balanced approach will expedite access while continuing to ensure the drugs we reach for each day provide the benefits we have come to expect.
Recommended reading: “IMPAKTER ESSAY: ANGELL OF EQUITY- QUESTIONING MOTIVES AND THE NEED FOR GLOBAL BIOETHICS TO REGULATE BIG PHARMA”